Introduction
Increasing use and complexity of interventional fluoroscopy
Determinants of radiation dose from interventional fluoroscopy
Radiation risks from interventional fluoroscopy
Strategies to optimize radiation exposure from interventional fluoroscopy
Physician-patient communication before and after interventional fluoroscopy
Dosimetry records and follow up
Education and training
Conclusion
Reference list
Introduction
Interventional fluoroscopy uses ionizing radiation to guide small
instruments such as catheters through blood vessels or other
pathways in the body. Interventional fluoroscopy represents a
tremendous advantage over invasive surgical procedures, because
it requires only a very small incision, substantially reduces the
risk of infection and allows for shorter recovery time compared
to surgical procedures. These interventions are used by a rapidly
expanding number of health care providers in a wide range of
medical specialties. However, many of these specialists have little
training in radiation science or protection measures.
The growing use and increasing complexity of these procedures
have been accompanied by public health concerns resulting from
the increasing radiation exposure to both patients and health care
personnel. The rise in reported serious skin injuries and the
expected increase in late effects such as lens injuries and
cataracts, and possibly cancer, make clear the need for information
on radiation risks and on strategies to control radiation
exposures to patients and health care providers. This guide
discusses the value of these interventions, the associated radiation
risk and the importance of optimizing radiation dose.
Back to Top
Increasing use and complexity of interventional fluoroscopy
In 2002, an estimated 657,000 percutaneous transluminal
coronary angioplasty (PTCA) procedures were performed in
adults in the United States. In addition, the rate of coronary
artery stent insertion doubled from 157 to 318 per 100,000
adults, aged 45-64, from 1996 to 2000 (CDC 2004). At the
same time, the complexity of interventional fluoroscopy has been
increasing rapidly. This is due to the development of new
devices and procedures, such as endografts for the treatment of
abdominal aortic aneurysms, the development of vertebroplasty,
kyphoplasty and uterine artery embolization, and increasing use
of fluoroscopic guidance during complex endoscopic biliary and
upper urinary tract procedures. As the complexity of these
procedures has increased, the dose to patients and health care
personnel has increased as well.
Back to Top
Determinants of radiation dose from interventional fluoroscopy
The radiation beam in interventional fluoroscopy procedures is typically
directed at a relatively small patch of skin for a substantial length of time.
This area of skin receives the highest radiation dose of any portion of the
patient's body. The dose to this skin area may be high enough to cause a
sunburn-like injury, hair loss, or in rare cases, skin necrosis (Mettler 2002).
Threshold doses for potential radiation effects with related time of onset are
presented below (ICRP 2000). The highest doses have been reported most
frequently as a result of PTCA, radiofrequency cardiac ablation procedures,
transjugular intrahepatic portosystemic shunts (TIPS) procedures and
embolization procedures in the brain (Koenig 2001).
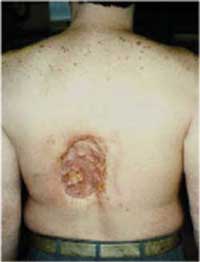 |
Appearance of radiation-induced skin injury approximately 18 to 21 months
following multiple coronary angiography and angioplasty procedures - evidence
of progressive tissue necrosis (Source: www.fda.gov/cdrh/rsnaii.html) |
Potential Clinical Effects of Radiation Exposures to the Skin and Eye Lens
| |
Effects |
Threshold dose (Gy) |
Time of onset |
| Skin |
Early transient erythema |
2 |
2-24 hours |
| Main erythema reaction |
6 |
~1.5 weeks |
| Temporary epilation |
3 |
~3 weeks |
| Permanent epilation |
7 |
~3 weeks |
| Dermal necrosis |
>12 |
>52 weeks |
| Eye |
Lens opacity (detectable) |
>1-2 |
>5 years |
| Lens/cataract (debilitating) |
>5 |
>5 years |
Source: ICRP, 2000
During a procedure, several major parameters influence dose:
-
Number of images taken
-
Fluoroscopy time, field size and overlap of fields (Miller 2002)
-
Tube filtration, generator voltage and current
-
Reduced-dose pulsed fluoroscopy versus continuous fluoroscopy (Wagner 2000)
-
Distance between the X-ray tube and the patient and between the patient and the
image receptor
-
Patient body habitus
Radiation dose is optimized when imaging is performed with the least amount of
radiation required to provide adequate image quality and imaging guidance.
Optimizing patient radiation dose also provides a direct benefit to the
operator and assistants: scattered radiation in the room is directly
proportional to the patient dose. If patient dose is reduced, so is the dose to
the operator.
Back to Top
Radiation risks from interventional fluoroscopy
The benefits of properly performed interventional fluoroscopy almost always
outweigh the radiation risk experienced by an individual. However, unnecessary
exposure to radiation can produce avoidable risk to both the patient and the
operator.
The short-term risk to patients is radiation-induced skin damage, which can
result from acute radiation doses of >= 2Gy. The extent of the skin injury may
not be known for weeks after the procedure. Repeated procedures increase the
risk of skin injury, because previous radiation exposure sensitizes the skin.
Long term effects include the potential risk of cancer. It is generally accepted
that there is probably no low dose "threshold" for inducing cancers, i.e. no
amount of radiation should be considered absolutely safe. Recent data from the
atomic bomb survivors (Pierce 2000) and medically irradiated populations
(UNSCEAR 2000) demonstrate small, but significant increases in cancer risk even
at the level of doses that are relevant to interventional fluoroscopy
procedures. The increased risk of cancer depends upon the age and sex of the
patient at exposure. Children are considerably more sensitive to radiation than
adults, as consistently shown in epidemiologic studies of irradiated
populations.
Health care providers are also at risk of radiation damage from chronic exposure
to radiation from these procedures. There are an increasing number of case
reports of skin changes on the hands and injuries to the lens of the eye in
operators and assistants (Faulkner 2001). Although cancer is uncommon, cancers
associated with radiation exposure in adults may include leukemia and breast
cancer (Yoshinaga 2004).
| Immediate |
Long-Term |
| Optimize dose to patient |
|
Use proper radiologic technique:
-
Maximize distance between x-ray tube and patient
-
Minimize distance between patient and image receptor
-
Limit use of electronic magnification
Control fluoroscopy time:
-
Limit use to necessary evaluation of moving structures
-
Employ last-image-hold to review findings
Control images:
-
Limit acquisition to essential diagnostic and documentation purposes
Reduce dose:
-
Reduce field size (collimate) and minimize field overlap
-
Use pulsed fluoroscopy and low frame rate
|
Include medical physicist in decisions
-
Machine selection and maintenance
Incorporate dose-reduction technologies and dose-measurement devices in equipment
Establish a facility quality improvement program that includes an appropriate
x-ray equipment quality assurance program, overseen by a medical physicist,
which includes equipment evaluation/inspection at appropriate intervals.
|
|
Minimize Dose to Operators and Staff |
|
Keep hands out of the beam
Use movable shields
Maintain awareness of body position relative to the x-ray beam:
-
Horizontal x-ray beam - operator and staff should stand on the side of the
image receptor
-
Vertical x-ray beam - the image receptor should be above the table
Wear adequate protection
-
Protective well-fitted lead apron
-
Leaded glasses
|
Improve ergonomics of operators and staff:
-
Train operators and staff in ergonomically good positioning when using
fluoroscopy equipment; periodicially assess their practice
-
Identify and provide the ergonomically best personal protective gear for
operators and staff
-
Urge manufacturers to develop ergonomically improved personal protective gear
-
Recommend research to improve ergonomics for personal protective gear
|
Back to Top
Strategies to optimize radiation exposure from interventional fluoroscopy
An important goal of all interventional fluoroscopy is
to achieve clinical success using the least amount of
radiation consistent with adequate imaging guidance.
However, most interventional procedures require high
quality images, long fluoroscopy time or both. Using
appropriate operating parameters for x-ray machines
will lower radiation doses to patients, and therefore to
operators and assistants as well. It is critically important
to adequately train operators and their assistants
to use equipment that provides acceptable image quality
along with the maximum possible dose-reduction,
and to have equipment regularly inspected and maintained.
Physicians, technologists, medical physicists,
fluoroscopy equipment manufacturers and medical and
governmental organizations share the responsibility to
optimize radiation doses to patients undergoing interventional
fluoroscopy.
Back to Top
Physician-patient communication before and after interventional fluoroscopy
Operators should always ask the patient about any
previous history of interventional fluoroscopy before
undertaking another procedure. It is important to
communicate the details of the procedure, patient
dose, and immediate and potential long-term health
effects to patients and their primary care providers.
Patients should be counseled on
radiation-related risks, as appropriate, along with the
other risks and benefits associated with the procedure.
If patients are likely to have multiple interventional
fluoroscopy procedures in a short period of time,
they should be informed if there is a possibility that
significant radiation exposures may accompany these
procedures and may cause potential short-term and
long-term radiation-related health effects.
After a procedure, the measured or
estimated radiation dose should be reviewed (Miller
2004), and appropriate steps should be taken to insure
adequate patient follow-up:
- Schedule a follow-up visit 30 days after the procedure
for all patients who received a radiation skin
dose of 2 Gy or more or a cumulative dose of 3 Gy
or more.
- Send the interventional fluoroscopy procedure
description, operative notes, doses and information
about possible short-term and long-term effects to
the patient's primary care provider.
- The patient and primary care physician should be
specifically requested to notify the operator if
observable skin effects occur.
Back to Top
Dosimetry records and follow up
Measure & record patient radiation dose:
- Record fluoroscopy time
- Record available measures - DAP (dose area product),
cumulative dose, skin dose
Inform patients who have received high doses to
examine the x-ray beam entrance site for skin erythema |
Develop methods to quantify late effects:
- Design medical records to clearly document the number
and types of interventional procedures received by the
patient
- Maintain a database of all patients with procedure and
dose information
- Review dose information to identify patients with high
doses (>2Gy) for follow up
- Establish procedures for follow-up, including skin
examination at 30 days
|
Back to Top
Education and training
Comprehensive training of operators in radiation biology, physics and safety:
- Attend high-quality courses or complete a self-training course given by appropriate professional societies; comply with
applicable state requirements
Monitor and improve performance of operator:
- Audit outcomes of procedures (including patient radiation dose) for each operator
- Share information learned in audits with operators and provide additional training as needed
- Provide annual radiation safety education for all operators
- Collaborate in clinical trials to identify best practices for optimizing doses to patients and minimizing doses to health
care providers
|
Back to Top
Conclusion
Interventional fluoroscopy is an increasingly important and valuable tool for treating disease, but it
is not without risk. It is important for the health care community, manufacturers and regulators to
work together to optimize patient radiation dose. Physicians must continuously think about optimizing
radiation dose to the patient. Used prudently and optimally, interventional fluoroscopy is
one of the valuable treatment modalities for a wide variety of diseases and disorders.
Back to Top
Reference list
Centers for Disease Control/National Center for Health Statistics, Health Care in America: Trends in Utilization, U. S. Department of
Health and Human Services, DHHS Pub No. 2004-1031, 2004.
Faulkner,K. and Vaño,E. Deterministic Effects in Interventional Radiology. Rad Prot Dosim 2001; 94:95-8.
International Commission on Radiological Protection. Avoidance of radiation injuries from medical interventional procedures. ICRP
Publication No. 85. Ann ICRP 2000;30:7-67.
Koenig TR, Wolff D, Mettler FA, Wagner LK. Skin injuries from fluoroscopically guided procedures . Am J Roentgenol 2001; 177:3-
20.
Mettler F, Koenig TR, Wagner LK, Kelsey CA. Radiation injuries after fluoroscopic procedures. Seminars Ultrasound, CT, MRI
2002; 23:428-42.
Miller DL, Balter S, Noonan PT, Georgia JD. Minimizing radiation-induced skin injury in interventional radiology procedures.
Radiology 2002; 225:329-36.
Miller DL, Balter S, Wagner LK, et al. Quality improvement guidelines for recording patient radiation dose in the medical record. J
Vasc Interv Radiol 2004; 15:423-9.
Pierce DA, Preston DL. Radiation-related cancer risks at low doses among atomic bomb survivors. Radiat Res 2000; 154:78-86.
Sources and Effects of Ionizing Radiation. United Nations Scientific Committee on the Effects of Atomic Radiation, UNSCEAR 2000
Report to the General Assembly, with Scientific Annexes, Volume II: Effects. New York: United Nations, 2000.
Wagner LK, Archer BR, Cohen J. Management of patient skin dose in fluoroscopically guided interventional procedures. J Vasc Interv
Radiol 2000; 11:23-33
Yoshinaga S, Mabuchi K, Sigurdson AJ, Doody MM, Ron E. Cancer risks among radiologists and radiologic technologists: Review of
epidemiologic studies. Radiology 2004; 233:313-21.
National Cancer Institute
Division o f Cancer Epidemiology and Genetics
Radiation Epidemiology Branch
6120 Executive Blvd., Suite 7047 MSC 7238
Rockville, MD 20852
dceg.cancer.gov
|
Society for Interventional Radiology
10201 Lee Highway, Suite 500
Fairfax, VA 22030
www.sirweb.org |
Back to Top
|