 |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
||||
| ||||||||||
|
|
|
|
Chlamydia Screening Among Sexually Active Young Female Enrollees of Health Plans --- United States, 1999--2001Chlamydia trachomatis infection is the most commonly reported sexually transmitted disease (STD) in the United States, with the highest rates among adolescent females and young women. Approximately 5%--14% of routinely screened females aged 16--20 years and 3%--12% of women aged 20--24 years are infected with chlamydia (1). Because up to 70% of chlamydial infections in women are asymptomatic, routine screening and treatment of infected persons is essential to prevent pelvic inflammatory disease, infertility, ectopic pregnancy, and perinatal infections. Since the 1990s, CDC, the U.S. Preventive Services Task Force, and several clinical organizations have recommended routine screening for chlamydial infection for all sexually active women aged <26 years and for pregnant women of all ages (1,2). To evaluate rates of chlamydia screening among sexually active young females, CDC analyzed 1999--2001 data from the Health Plan Employer Data and Information Set (HEDIS®) reported by commercial and Medicaid health insurance plans. This report summarizes the results of that analysis, which determined that screening rates were low despite slight increases in screening covered both by commercial and Medicaid plans during 1999--2001. Increased screening by health-care providers and coverage of screening by health plans will be necessary to reduce substantially the burden of chlamydial infection in the United States. HEDIS includes voluntarily reported performance measures of health plans and is maintained by the National Committee for Quality Assurance (NCQA), a private, not-for-profit organization that monitors the quality of health plans. HEDIS allows health insurance purchasers and consumers to compare health plan performance and enables health plans to benchmark their performance. During 1999--2001, a total of 335 commercial health maintenance organizations (HMOs) and point-of-service (POS) plans and 92 Medicaid HMO and POS plans reported chlamydia screenings. These data accounted for 83% of enrollees in commercial HMO and POS plans and up to 30% of enrollees in Medicaid HMO and POS plans in the United States during this period. Since 1999, NCQA has measured chlamydia screening rates of sexually active female enrollees in these health plans by using medical claims and pharmacy data. The denominator represents the number of sexually active female enrollees aged 16--26 years who were continuously enrolled during the preceding calendar year. Being sexually active was defined as receipt of a contraceptive prescription or submission of a medical claim associated with pregnancy, contraceptives, STDs, or Papanicolaou (Pap) test during the preceding year. The numerator represents the number of eligible female enrollees who had a claim for chlamydia tests. Mean chlamydia screening rates were weighted to account for the differences in the number of sexually active female enrollees aged 16--26 years across health plans. Among sexually active female enrollees aged 16--26 years in commercial plans, 20% were screened for chlamydia in 1999, 25% in 2000, and 26% in 2001. Among enrollees aged 16--26 years in Medicaid plans, screening rates were 28% in 1999, 36% in 2000, and 38% in 2001. Among enrollees aged 16--20 years in commercial plans, 22% were screened in 1999, 27% in 2000, and 28% in 2001 (Figure). Among enrollees aged 16--20 years in Medicaid plans, 27% were screened in 1999, 35% in 2000, and 38% in 2001. Of commercial plan enrollees aged 21--26 years, 19% were screened in 1999, 24% in 2000, and 25% in 2001. Of Medicaid plan enrollees aged 21--26 years, 28% were screened in 1999, 36% in 2000, and 38% in 2001. Reported by: S Shih, MPH, S Scholle, DrPH, National Committee for Quality Assurance, Washington, DC. K Irwin, MD, G Tao, PhD, C Walsh, DrPH, Div of STD Prevention, National Center for HIV, STD, and TB Prevention; W Tun, PhD, EIS Officer, CDC. Editorial Note:Despite national guidelines recommending routine chlamydia screening (1,2), the data in this report suggest that screening rates remain low among enrollees in both commercial and Medicaid plans. These rates are lower than rates for all other women's health services measured by HEDIS, including Pap tests to screen for cervical cancer (61% in Medicaid and 80% in commercial plans in 2001) (3). Chlamydia screening rates might be higher in Medicaid than in commercial plans because of health-care providers' beliefs that Medicaid patients are at higher risk for STDs. Low screening rates in both commercial and Medicaid plans might result from certain system, provider, and patient factors. System factors include 1) lack of availability or coverage of urine-based screening tests in certain health plans, which would eliminate the need for a pelvic examination; 2) insufficient feedback and reminder systems about screening; and 3) inadequate organizational commitment to increase the availability of this preventive service. Provider factors include 1) lack of awareness of high chlamydia prevalence in adolescent females and young women and among commercial plan enrollees (4); 2) misperceptions that adolescent patients are not sexually active (4) or that commercially insured patients are not at risk for chlamydial infection; 3) discomfort with discussing or lack of time for assessing sexual activity and offering chlamydia screening; and 4) lack of knowledge of the availability of urine-based chlamydia screening tests. Patient factors include 1) the stigma associated with STDs; 2) lack of awareness of the high prevalence, asymptomatic nature, and serious complications of chlamydial infection; 3) the presence of parents during the examinations of adolescents, which precludes confidential sexual risk assessment; and 4) fears about breaches of confidentiality regarding sexual health services or diagnoses noted in medical records or bills (5). The findings in this report are subject to at least two limitations. First, HEDIS data reflect screenings reported by HMO and POS plans that covered only approximately 30% of U.S. residents in 2001. Second, HEDIS estimates might underestimate or overestimate actual screening rates for these health plan enrollees. HEDIS depends on routinely collected administrative data to facilitate data collection within plans and allow comparison across plans. However, if a substantial proportion of sexually inactive enrollees had claims for pregnancy tests or oral contraceptives for reasons not related to sexual activity, or if medical claims did not identify all chlamydia tests ordered, HEDIS data would underestimate actual screening rates. Overestimation might occur if a substantial proportion of sexually active enrollees lacked claims for pregnancy, contraceptives, STDs, or Pap tests that would classify them as sexually active in administrative data (5), or if the measure's numerator included claims for chlamydia tests used to diagnose illness in symptomatic patients (5). Overestimation also might result if health plans that perform well on the chlamydia screening measure are more likely to report their results to NCQA than those that do not perform as well. Continued evaluation is needed of how well administrative data used for HEDIS measures reflect actual practice. The findings in this report highlight the need for interventions to increase chlamydia screening, improve quality of care, and reduce the estimated $249 million direct medical costs of chlamydia and its sequelae for adolescents and young adults (6). Interventions are especially important in commercial plans, given that two thirds of women of reproductive age (15--44 years) in the United States are commercially insured (7) and only 13% of chlamydial infections in the CDC surveillance system are reported by public STD clinics (8). System-level interventions in large commercial plans have substantially increased chlamydia screening rates of sexually active young women within 2 years (9,10). One intervention increased screening from 5% to 65% by 1) informing providers about high chlamydia prevalence, 2) implementing procedures allowing adolescents some encounter time without parents, and 3) providing urine tests and monthly provider feedback on screening rates (9). Another intervention, which included "championing" of screening by health-plan leaders and routine placement of chlamydia specimen collection materials next to Pap test collection kits, increased screening from 61% to 83% (10). Such system-level interventions should complement provider and patient education. In addition, including chlamydia screening as one of the HEDIS measures used to accredit health plans by NCQA might provide motivation to increase screening. Acknowledgment This report is based, in part, on data contributed by 427 health plans reporting HEDIS® data to NCQA. References
Figure 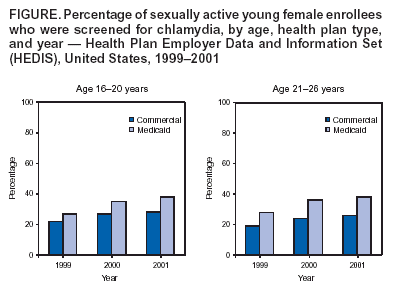 Return to top.
Disclaimer All MMWR HTML versions of articles are electronic conversions from ASCII text into HTML. This conversion may have resulted in character translation or format errors in the HTML version. Users should not rely on this HTML document, but are referred to the electronic PDF version and/or the original MMWR paper copy for the official text, figures, and tables. An original paper copy of this issue can be obtained from the Superintendent of Documents, U.S. Government Printing Office (GPO), Washington, DC 20402-9371; telephone: (202) 512-1800. Contact GPO for current prices. **Questions or messages regarding errors in formatting should be addressed to mmwrq@cdc.gov.Page converted: 10/28/2004 |
|||||||||
This page last reviewed 10/28/2004
|