|
HIV transmission from mother to child during pregnancy, labor and delivery, or breastfeeding is called perinatal transmission. Research published in 1994 showed that zidovudine (ZDV) given to pregnant women infected with HIV and their newborns reduced the risk for this type of HIV transmission [1]. Since then, the testing of pregnant women and treatment for those who are infected have resulted in a dramatic decline in the number of children perinatally infected with HIV. However, much work remains to be done: about 100–200 infants in the United States are infected with HIV annually. Many of these infections involve women who were not tested early enough in pregnancy or who did not receive prevention services.
Perinatal HIV transmission is the most common route of HIV infection in children and is now the source of almost all AIDS cases in children in the United States. Most of the children with AIDS are members of minority races/ethnicities [2].
STATISTICS
HIV/AIDS in 2005
The following bullets are data from the 33 states with long-term, confidential name-based HIV reporting. For a list of the 33 states, see the box at the end of this fact sheet.
- HIV/AIDS was diagnosed for an estimated 142 children less than 13 years old who had been infected with HIV perinatally [2].
- An estimated 6,051 persons who had been infected with HIV perinatally were living with HIV/AIDS at the end of 2005 [2].
- Of the perinatally infected persons living with HIV/AIDS at the end of 2005, an estimated 66% were black (not Hispanic or Latino), and an estimated 20% were Hispanic/Latino [2].
AIDS in 2005
- Of the estimated 68 children for whom AIDS was diagnosed during 2005, an estimated 67 had been infected with HIV perinatally [2].
- An estimated 46 persons with AIDS who had been infected with HIV perinatally died in
2005 [2].
- Since the beginning of the epidemic, AIDS has been diagnosed for an estimated 8,460 children who were infected perinatally. Of those, an estimated 4,800 (57%) had died [2].
- Over the course of the epidemic, the number of AIDS cases associated with perinatal transmission has decreased dramatically. This decrease is largely due to the increased identification of women infected with HIV and timely interventions to prevent perinatal transmission [3].
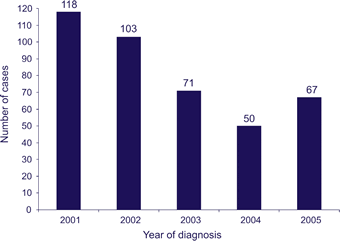
AIDS cases due to the perinatal transmission of HIV infection, by year of diagnosis, 2001–2005, United States [2]
Race/ethnicity of children (<13 years) with AIDS diagnosed during 2005 (includes all children with a diagnosis of AIDS, not just those who contracted HIV perinatally)

Note. Includes children of unknown race or multiple races. Because the total is less than 100, this graph shows numbers, not percentages. No cases of AIDS were diagnosed among American Indian/Alaska Native children.
RISK FACTORS AND BARRIERS TO PREVENTION
Lack of Awareness of HIV Serostatus
The main risk factor, which is also a barrier to the prevention of perinatal HIV transmission, is lack of awareness of HIV status among pregnant women.
- Because approximately 25% of all people infected with HIV do not know their HIV status [4], many women who are infected with HIV may not know they are infected. This is why CDC has recommended routine, opt-out1 HIV testing for all pregnant women [5]. If women are tested early in their pregnancy, those who are infected can be given therapy to improve their own health and reduce the risk of transmitting HIV to the baby.
- In the United States, without antiretrovial therapy, approximately 25% of pregnant women infected with HIV will transmit the virus to their child [1].
Uneven HIV Testing Rates
Recent CDC studies found that HIV testing rates for pregnant women varied widely and that a relatively high proportion of women of childbearing age were unaware that treatment is available to reduce the risk for perinatal transmission [6,
7]. In a 2002 study of HIV testing in the United States, 31% of the 748 women who had recently been pregnant reported that they had not been tested during prenatal care [8]. Continued efforts are needed to ensure that all women know their HIV status as early as possible in pregnancy.
- Because of prenatal testing, most HIV-infected women know they are infected before they give birth [3]. Still, testing rates in the United States remain uneven: 18% of the women in another study were not tested until after childbirth [9].
- State HIV testing rates differ, depending on the testing approach used. For example, rates for states using the opt-in2 approach ranged from 25% to 69%. The opt-out approach results in higher testing rates [6]. CDC recommends the opt-out approach [5], but in many prenatal settings, it has not been implemented. CDC is working with state and local health departments and national organizations to increase the rates of HIV testing among pregnant women.
PREVENTION
To reduce further the incidence of HIV infection, CDC announced a new initiative,
Advancing HIV Prevention (AHP),
in 2003 [10]. This initiative comprises 4 strategies: making HIV testing a routine part of medical care, implementing new models for diagnosing HIV infections outside medical settings, preventing new infections by working with HIV-infected persons and their partners, and further decreasing perinatal HIV transmission.
In 2006, CDC published “Revised Recommendations for HIV Testing of Adults, Adolescents, and Pregnant Women in Health-Care Settings” [5]. To further reduce the number of children who are infected with HIV perinatally, these recommendations called for routine opt-out HIV screening for all pregnant women, with repeat HIV screening in the third trimester for women who meet 1 or more of 4 criteria (for example, women at high risk and women who receive health care in jurisdictions with elevated rates of HIV infection among women). Women whose HIV status is unknown at the time of labor should be offered opt-out screening with a rapid HIV test.
In support of these recommendations, CDC developed a social marketing campaign—One Test. Two Lives. —with the goal of ensuring that all women are tested for HIV early in their pregnancy. The campaign provides quick access to a variety of resources for health care providers, along with materials for their patients, to encourage universal voluntary prenatal testing for HIV. Information on this campaign can be found at
http://www.cdc.gov/1test2lives.
Already, perinatal HIV prevention has saved lives.
- The number of children with a diagnosis of AIDS who had been perinatally exposed to HIV declined from 118 in 2001 to 67 in 2005 [2]. The number of infants infected with HIV through perinatal transmission decreased from an estimated peak of 1,650 HIV-infected infants born in 1991 [3] to 96–186 infants born in 2004 [11].
- Antiretroviral therapy administered to the mother during pregnancy, labor and delivery, and then to the newborn, as well as elective cesarean section for women with high viral loads (more than 1,000 copies/ml), can reduce the rate of perinatal HIV transmission to 2% or less [12]. If medications are started during labor and delivery, the rate of perinatal
transmission can still be decreased to
less than 10% [13].
CDC funds 15 state and local health departments to conduct perinatal HIV prevention programs. The following are examples of CDC-funded perinatal HIV prevention programs:
- Comprehensive social marketing campaigns in New York to encourage women to be tested for HIV and to get early prenatal care [14]
- Tracking and surveillance programs in Louisiana to identify HIV-infected pregnant women who are not receiving medical care and connect these women to health care
resources [15]
- Outreach programs in Florida for women in nontraditional settings, including jails [15]
- Intensive provider education programs in New Jersey to disseminate the state standard of care for perinatal HIV prevention, educate providers about interventions for perinatal prevention, and implement rapid HIV testing for women whose HIV status is unknown at the time of labor and delivery
- Technical assistance to hospitals in Illinois to increase readiness and compliance with the Illinois Perinatal HIV Prevention Act [16]
- Regional strategic planning workshops supported by CDC-funded national organizations to help hospitals implement rapid HIV testing for women in labor whose HIV status is unknown [17]
1 Opt-out HIV testing:
women are told that an HIV test will be included in the standard group of prenatal tests but that they may decline HIV testing.
2 Opt-in HIV testing: women are provided pretest counseling and must specifically
consent to an HIV test.
Understanding HIV and AIDS Data
AIDS
surveillance: Through a uniform system, CDC receives reports of AIDS cases from all US states and dependent areas. Since the beginning of the epidemic, these data have been used to monitor trends because they are representative of all areas. The data are statistically adjusted for reporting delays and for the redistribution of cases initially reported without risk factors. As treatment
has become more available, trends in new AIDS diagnoses no longer accurately represent trends in new HIV infections; these data now represent persons who are tested late in the course of HIV infection, who have limited access to care, or in whom treatment has failed.
HIV surveillance: Monitoring trends in the HIV
epidemic today requires collecting information on HIV cases that have
not progressed to AIDS. Areas with confidential name-based HIV infection reporting requirements
use the same uniform system for data collection
on HIV cases as for AIDS cases. A total of 33 states
(Alabama, Alaska, Arizona, Arkansas, Colorado, Florida,
Idaho, Indiana, Iowa, Kansas, Louisiana, Michigan,
Minnesota, Mississippi, Missouri, Nebraska, Nevada,
New Jersey, New Mexico, New York, North Carolina,
North Dakota, Ohio, Oklahoma, South Carolina,
South Dakota, Tennessee, Texas, Utah, Virginia, West
Virginia, Wisconsin, and Wyoming) have collected
these data for at least 5 years, providing sufficient data
to monitor HIV trends and to estimate risk behaviors for
HIV infection.
HIV/AIDS: This term is used to refer to 3 categories of diagnoses collectively: (1) a diagnosis of HIV infection (not AIDS), (2) a diagnosis of HIV infection and a later diagnosis of AIDS,
and (3) concurrent diagnoses of HIV infection and AIDS. |
REFERENCES
- Connor EM, Sperling RS, Gelber R, et al. Reduction of maternal-infant transmission of human immunodeficiency virus type with zidovudine treatment.
New England Journal of Medicine 1994;331:1173–1180.
- CDC.
HIV/AIDS Surveillance Report, 2005. Vol. 17.
Rev. ed. Atlanta: US Department of Health and Human Services, CDC;
2007:1–54.
- Lindegren ML, Byers RH, Thomas P, et al. Trends in perinatal transmission of HIV/AIDS in the United States.
JAMA 1999;282:531–538.
- Marks G, Crepaz N, Janssen RS. Estimating sexual transmission of HIV from persons aware and unaware that they are infected with the virus in the USA.
AIDS 2006;20(10):1447–1450.
- CDC.
Revised recommendations for HIV testing of adults, adolescents, and pregnant women in health-care settings.
MMWR 2006;55(RR-14):1–17.
- CDC.
HIV testing among pregnant women―United States and Canada, 1998–2001.
MMWR
2002;51:1013–1016.
- Anderson JE, Ebrahim S, Sansom S. Women’s knowledge about treatment to prevent mother-to-child human immunodeficiency virus transmission.
Obstetrics and Gynecology 2004;103:165–168.
- Anderson JE, Sansom S. HIV testing among U.S. women during prenatal care: findings from the 2002 National Survey of Family Growth.
Maternal and Child Health Journal 2006;10(5):413–417.
- Aynalem G, Mendoza P, Mascola L, Frederick T. Trends and associated factors in timing of maternal HIV status identification: implications for preventing perinatal HIV/AIDS infection. National HIV Prevention Conference; August 2003; Atlanta. Abstract M2-B0303.
- CDC.
Advancing HIV Prevention: New Strategies for a Changing Epidemic—United States, 2003.
MMWR 2003;52(15):329–332.
- McKenna MT, Hu X. Recent trends in the incidence and morbidity associated with perinatal human immunodeficiency virus infection in the United States.
American Journal of Obstetrics and Gynecology 2007;197(3)(suppl 1):S10–S16.
- Cooper ER, Charurat M, Mofenson LM, et al. Combination antiretroviral strategies for the treatment of pregnant HIV-1–infected women and prevention of perinatal HIV-1 transmission.
Journal of Acquired Immune Deficiency Syndromes 2002;29(5):484–494.
- Wade NA, Birkhead GS, Warren BL, et al. Abbreviated regimens of zidovudine prophylaxis and perinatal transmission of the human immunodeficiency virus.
New England Journal of Medicine 1998;339(20):1409–1414
- Doyle PA, Rogers P, Gerka M, et al. Implementation of a comprehensive model for recruiting pregnant women at risk for HIV and late or no prenatal care. National HIV Prevention Conference; August 2003; Atlanta. Abstract T1-C1002.
- Clark J, Sansom S, Simpson BJ, et al. Promising strategies for preventing perinatal HIV transmission: model programs from three states.
Maternal and Child Health Journal 2006;10(4):367–373.
- Bryant Borders AE, Eary RL, Olszewski Y, et al. Ready or not—intrapartum prevention of perinatal HIV transmission in Illinois.
Maternal and Child Health Journal 2007;11(5):485–493.
- Burr CK, Lampe MA, Gross E, Clark J, Jones R. A strategic planning approach to influencing hospital practice regarding rapid HIV testing in labor and delivery. Annual Meeting of the American Public Health Association; 2007; Washington DC. Abstract 161680.
|