| |
     |
< Previous | Home | Next >
Chapter
18
Overview TOP Doesn't the Guide itself provide sufficient information about HIV care? At a pace unlike that in any other field, rapid change characterizes the field of clinical HIV medicine. Fortunately, opportunities to stay current with the fast-paced changes in science and practice are available through a variety of sources. What kinds of resources are available for keeping up-to-date? One approach to identifying educational resources for providers is to consider them an expanding circle of information sources, starting at the local level, and finally reaching the globally available web of information on the Internet. Resources can also be grouped by type of information delivery:
What kind of standards are available to assure that HIV providers are keeping up-to-date? Professional associations and State governments have developed policies defining HIV specialists that specify the number of patients that providers should directly manage in order to qualify for this experience-driven classification, reinforcing through regulations and requirements the simple notion that providers need to keep current in order to provide good care. See last section, Integrating HIV Specialty into Practice, for details. Human Resources TOP How do you identify what's available in your own community? The single
most important step in obtaining current information is to identify
local resources. The first step is to determine whether any HIV
experts are practicing nearby who provide care to with HIV in the
community. HIV specialists are an important source of information
— not only about clinical practice, but also about educational
opportunities in the area. Local hospitals or clinics may offer
grand rounds on topics in HIV clinical care or continuing education
programs. Local infectious disease societies or HIV medical associations
may sponsor meetings at which new information is disseminated. Every
region in the United States is targeted by a regional AIDS Education
and Training Center (AETC), funded by the HIV/AIDS Bureau (HAB)
of the Health Resources and Services Administration (HRSA), that
offers a menu of educational programs designed to fit the specific
needs of practicing providers, including physicians, mid-level practitioners,
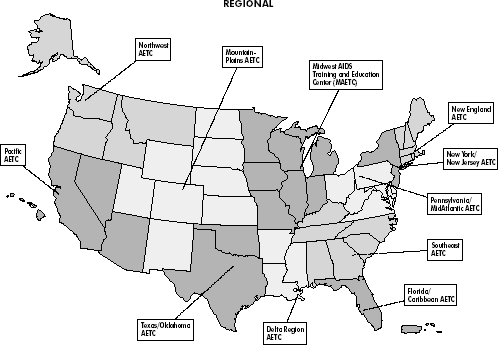
nurses, and dentists (see Figure 18-1). Figure
18-1. AIDS Education and Training Centers
Are AIDS conferences useful for providers who are not HIV experts? A number of national conferences provide opportunities to obtain cutting-edge information (see Table 18-1). The range of offerings usually meets the needs of providers just learning about HIV as well as providers who are already HIV experts.
What if you practice in a remote area? In remote geographic areas, the nearest HIV expert may actually be far away and attendance at conferences and meetings may not be feasible. In this situation, the regional AETC can be contacted to determine how to obtain direct educational programming. When distance prevents on-site attendance at educational programs, newer technologies may enable long distance participation. Satellite broadcasting and down-linking to local facilities may be available and has been a useful approach in various parts of the United States. Distance learning and web-based information also provide important sources of education when other programming is unavailable. Many sessions are videotaped or audiotaped. Videocassettes and audiocassettes may be distributed or purchased for a modest price. Is clinical consultation possible even if you are not affiliated with an HIV specialty practice? In areas of the country with no HIV clinical experts, a number of consultative and co-management options are available through the AETCs or statewide education initiatives to assure that patient care is of the highest quality. Informal discussions with experienced providers in the region are probably the easiest way to access expertise, especially since these providers may be available for formal clinical consultation when decisions are made about ART, such as when to initiate, modify, or discontinue therapy. Clinical consultations are available not only through the regional AETCs, but also from the National HIV Clinical Consultation Center, based at the University of California San Francisco (UCSF). This service provides a "warmline" — a toll-free phone number staffed from 6:00 a.m. to 5:00 p.m. PST by physicians, nurse practitioners, and pharmacists who are available to answer providers' questions. During other times, or when the phone line is busy, voicemail messages can be left and calls returned. The HIV experts discuss options with callers, presenting pros and cons of various approaches with the goal of improving the capability of the provider to manage the current situation and others like it. The Center also refers callers to their local resources for expertise, consultation and training. National
HIV/AIDS Clinical Consultation Written Resources TOP What books and journals are most useful for primary care providers? Although a basic textbook of HIV/AIDS medicine provides a basic reference of core knowledge, it becomes outdated nearly as quickly as it is published, particularly in relation to ART. Small books such as the Pocket Guide included in this guide contain quick reference materials, are more frequently updated, and provide summaries that can be useful at the point of care. Other books provide specialized information related to the care of specific groups of persons with HIV. For example, A Guide to the Clinical Care of Women with HIV offers an excellent comprehensive overview of issues pertaining to the care of women, with useful tables, photographs, and practical information for the provider. Most major journals include articles about HIV. Clinical trials and review articles periodically appear in the major internal medicine journals. Two important peer-reviewed HIV-specific journals, AIDS and JAIDS (Journal of the Acquired Immune Deficiency Syndromes and Human Retrovirology), include studies and review articles in the domains of basic science, epidemiology, clinical care, and HIV prevention. Other regularly published bulletins and journals offer review articles on basic aspects of clinical management that are useful summaries for the primary HIV care provider. The Johns Hopkins HIV Report provides summaries of current issues and controversies in HIV care authored by experts from the Hopkins HIV Service. Question and answer sessions with experts are often included as part of these publications. See Table 18-2 for a list of recommended publications. Also, a comprehensive list of HIV professional journals can be found online (accessed 3/04).
Can journal articles be accessed on the internet? To keep up with all of the HIV journals is impossible, especially when a practice is not exclusively devoted to HIV care. Several websites post information about newly published articles and can easily be scanned to seek relevant or noteworthy information (see Table 18-3). Medscape, which has a specific section dedicated to HIV, and HIVInSite are two good sources of news. An abstract of almost any article can be retrieved through the National Library of Medicine's website at PubMed. A useful list of websites, references and news may also be found at Medline Plus. The Kaiser Daily HIV/AIDS Report offers a daily news summary that includes both newspaper articles and major clinical or scientific releases that anyone can subscribe to by registering at the website. The Aegis website links to news summaries that can be quickly accessed to obtain the desired summary. Are there guidelines for HIV care? The Department of Health and Human Services has sponsored several guidelines panels composed of HIV clinical experts to develop evidence-based and consensus-driven practice recommendations for the provision of HIV care. These guidelines are updated regularly, and are posted on the official website of AIDSInfo, a service of the U.S. Department of Health and Human Services. Currently available Federal guidelines address the following topics:
New York State has sponsored an HIV Guidelines Program since 1985 through which independent guidelines are developed that specifically target frontline providers and contain concise recommendations for primary care physicians, nurse practitioners, and physician assistants. In addition to guidelines for adults and children, other guidelines specifically address mental health and oral health for persons with HIV. These guidelines, along with information about implementation strategies, including best practices, quality improvement methods, and success stories, can be found online. Electronic and Web-Based Resources TOP Which web-based resources are most useful? Numerous websites provide useful information about HIV. While it is beyond the scope of this chapter to provide a comprehensive listing of all HIV-related websites, Table 18-3 is a partial listing of some particularly useful ones. Websites in the Search Engines category allow the user to enter a topic of interest and obtain a list of other websites or resources from which to choose. There are search engines that are general as well as medical. Websites in the Resource Listings category provide lists of HIV resources, including agencies, other websites, and informational materials. The General HIV Resources category contains some of the websites that are most useful when specific HIV information is being sought. One important example is the database of antiretroviral drug interactions that is part of the HIV InSite website. The HIV CME websites provide continuing medical education and award CME credits, usually at no cost. The Specific HIV Topics category lists some of the websites addressing focused issues related to HIV care, such as drug dependency and treatment adherence. Websites targeting consumers enable them to directly access scientific and clinical information and to pose questions to experts. These websites empower patients by helping them to better understand their disease and its manifestations and by enabling them to advocate for their own health and to more fully participate in decisionmaking about their care. See Table 2-1, Information Resources for Patients, in Chapter 2. Thinking ahead: can personal digital assistants (PDAs) help you keep up? A revolution in healthcare information technology has begun that brings information resources directly to the provider at the point of care, whether at the bedside or during the clinic visit. Mobile computing through handheld devices, such as personal digital assistants (PDAs), are now available and have begun to change the practice of medicine by facilitating capture of data and retrieval of information. PDAs (eg, Palm, Pocket PC, Visor) are now used as clinical tools for reference, prescribing, coding and patient education (see Table 18-4).
Currently, the greatest advantage of carrying a PDA is having medical resources at your fingertips. Through a function that uses a cradle to connect with a website via a personal computer, the provider's PDA can "synch" with a master database that is maintained and updated regularly. Transfer of information is easily accomplished with PDAs through "beaming." By pointing the PDA at another PDA and tapping on the appropriate prompts, data are quickly transported into the other PDA database. Similarly, information can be beamed to a printer, which is a particularly useful feature for quickly printing patient information or prescriptions. As PDA technology rapidly evolves, the utility and efficacy of handheld computing will similarly expand. Potential new uses of PDA technology include portable access to MEDLINE, full text journal articles, information searches, comprehensive information storage, and point-of-care access to guidelines, algorithms, and other decisionmaking tools to enhance the quality of care. PDA versions of patient tracking systems and coding references have also been developed. Ultimately, PDAs will be used in conjunction with electronic medical record systems, with information being "beamed" between the two systems. This powerful application of PDA technology will permit comprehensive individualized patient data files that can include current and past medical information, laboratory data, and even reminders for providers to perform periodic preventive health or monitoring tests. Providers who have not already taken the first step, purchasing and using a PDA, should become acquainted with this important new technology as an important source of clinical information and aid to patient management (see Table 18-5).
Integrating HIV Specialty into Practice TOP Making it stick: how can you integrate new information into clinical practice? Numerous resources at the fingertips of providers enable them to obtain up-to-the-minute information about new developments or management strategies for HIV care. However, even the best-educated provider cannot assure that quality of care will be achieved through access to the most recent standards and current information unless the system in which care is provided has been adapted to integrate that information. Strategies for developing and sustaining systems to support information can be implemented at the local level through individual actions and through quality improvement programs. A variety of resources provide assistance in successfully integrating current information into HIV care. Most notably, the decision support framework of the chronic care model developed by the University of Washington has been used to improve care delivered by Ryan White CARE Act-funded clinics (see Figure 1-1 in Chapter 1). Quality improvement strategies based on this model include the following principles:
One example of the application of these strategies is conducting chart audits in order to benchmark practices and feed the information back to providers. Other examples are using flow sheets or checklists to embed guidelines into practice and developing simplified versions of guidelines for providers and patients. The most successful strategies to incorporate guidelines into systems of care are those that include reminders at the point of care or decisionmaking. An important rule of thumb is that multiple interventions work better than just one. For more information on quality improvement, see Chapter 17. How do you develop the experience needed to qualify as an HIV specialist? Multiple studies show better outcomes when providers managing patients have expertise in HIV (see Table 18-6). In the absence of a formally recognized subspecialty society devoted to HIV medicine, government agencies, professional societies, and academic institutions have developed definitions of HIV specialization in order to develop policies, standards, and regulations, and to monitor the quality of care provided to persons with HIV (see Table 18-7). Definitions of HIV specialists generally focus on two major areas, experience and HIV CME credits, and also require that experience be current and that knowledge be updated annually. Generally, requirements for experience in the care of patients with HIV range from 10 to 20 patient-years of experience. All definitions emphasize currency of experience and education, given the rapid pace at which HIV clinical management standards change.
|
|||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
![]()
Top
| Home | HRSA
| HHS |
Disclaimer | Accessibility
| Privacy | Download
Adobe Reader| | Freedom of Information
Act