What Is Heart Valve Disease?
Heart valve disease is a condition in which one or
more of your heart valves don't work properly. The heart has four valves: the
tricuspid (tri-CUSS-pid), pulmonary (PULL-mun-ary), mitral (MI-trul), and
aortic (ay-OR-tik) valves.
These valves have tissue flaps that open and close
with each heartbeat. The flaps make sure blood flows in the right direction
through your heart's four chambers and to the rest of your body.
Healthy Heart Cross-Section
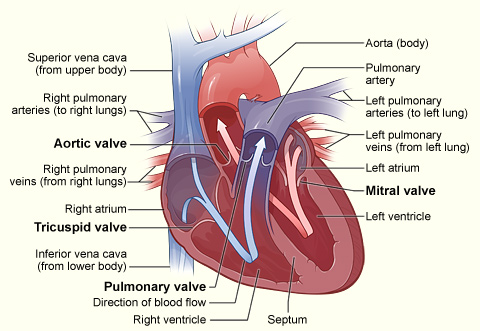
The illustration shows a
cross-section of a healthy heart, including the four heart valves. The blue
arrow shows the direction in which oxygen-poor blood flows from the body to the
lungs. The red arrow shows the direction in which oxygen-rich blood flows from
the lungs to the rest of the body.
Birth defects, age-related changes, infections, or
other conditions can cause one or more of your heart valves to not open fully
or to let blood leak back into the heart chambers. This can make your heart
work harder and affect its ability to pump blood.
Overview
How the Heart Valves Work
At the start of each heartbeat, blood returning from
the body and the lungs fills the heart's two upper chambers. The mitral and
tricuspid valves are located at the bottom of these chambers. As the blood
builds up in the upper chambers, these valves open to allow blood to flow into
the lower chambers of your heart.
After a brief delay, as the lower chambers begin to
contract, the mitral and tricuspid valves shut tightly. This stops blood from
flowing backward.
As the lower chambers contract, they pump blood
through the pulmonary and aortic valves. The pulmonary valve opens to allow
blood to flow from the right lower chamber into the pulmonary artery. This
artery carries blood to the lungs to get oxygen.
At the same time, the aortic valve opens to allow
blood to flow from the left lower chamber into the aorta. This aorta carries
oxygen-rich blood to the body. As the contraction ends, the pulmonary and
aortic valves shut tightly. This stops blood from flowing backward into the
lower chambers.
For more information on how the heart pumps blood,
see the animation in the "Heart
Contraction and Blood Flow" section of the Diseases and Conditions Index
article on How the Heart Works.
Heart Valve Problems
Heart valves can have three basic kinds of problems:
- Regurgitation (re-GUR-ji-TA-shun), or backflow,
occurs when a valve doesn’t close tightly. Blood leaks back into the
chamber rather than flowing forward through the heart or into an artery.
- In the United States, backflow
is most often due to prolapse. "Prolapse" is when the flaps of the valve flop
or bulge back into an upper heart chamber during a heartbeat. Prolapse mainly
affects the
mitral
valve, but it can affect the other valves as well.
- Stenosis (ste-NO-sis) occurs when the flaps of a
valve thicken, stiffen, or fuse together. This prevents the heart valve from
fully opening, and not enough blood flows through the valve. Some valves can
have both stenosis and backflow problems.
- Atresia (a-TRE-ze-AH) occurs when a heart valve
lacks an opening for blood to pass through.
You can be born with heart valve disease or you can
acquire it later in life. Heart valve disease that develops before birth is
called a congenital (kon-JEN-i-tal) valve disease. Congenital heart valve
disease can occur alone or with other
congenital
heart defects.
Congenital heart valve disease usually involves
pulmonary or aortic valves that don't form properly. These valves may not have
enough tissue flaps, they may be the wrong size or shape, or they may lack an
opening through which blood can flow properly.
Acquired heart valve disease usually involves the
aortic or mitral valves. Although the valve is normal at first, disease can
cause problems to develop over time.
Both congenital and acquired heart valve disease can
cause stenosis or backflow.
Outlook
Many people have heart valve defects or disease but
don't have symptoms. For some people, the condition will stay largely the same
over their lifetime and not cause any problems.
For other people, the condition will worsen slowly
over time until symptoms develop. If not treated, advanced heart valve disease
can cause
heart
failure, stroke, blood clots, or sudden death due to
sudden
cardiac arrest.
Currently, no medicines can cure heart valve
disease. However, lifestyle changes and medicines can relieve many of the
symptoms and problems linked to heart valve disease. They also can lower your
risk of developing a life-threatening condition, such as stroke or sudden
cardiac arrest. Eventually, you may need to have your faulty heart valve
repaired or replaced.
Some types of congenital heart valve disease are so
severe that the valve is repaired or replaced during infancy or childhood or
even before birth. Other types may not cause problems until you're middle-aged
or older, if at all.
Other Names for Heart Valve Disease
- Aortic regurgitation
- Aortic stenosis
- Aortic sclerosis
- Aortic valve disease
- Bicuspid aortic valve
- Congenital
heart defect
- Congenital valve disease
- Mitral regurgitation
- Mitral stenosis
- Mitral valve disease
- Mitral
valve prolapse
- Pulmonic regurgitation
- Pulmonic stenosis
- Pulmonic valve disease
- Tricuspid regurgitation
- Tricuspid stenosis
- Tricuspid valve disease
What Causes Heart Valve Disease?
Heart conditions and other disorders, age-related
changes, rheumatic fever, and infections can cause acquired heart valve
disease. These factors change the shape or flexibility of once-normal
valves.
The cause of congenital heart valve defects isn't
known. These defects occur before birth as the heart is forming. Congenital
heart valve defects can occur alone or with other types of
congenital
heart defects.
Heart Conditions and Other Disorders
Heart valves can be stretched and distorted by:
- Damage and scar tissue due to a
heart
attack or injury to the heart.
- Advanced
high
blood pressure and
heart
failure. These conditions can enlarge the heart or the main arteries.
- Narrowing of the aorta due to the buildup of a
fatty material called plaque (plak) inside the artery. The aorta is the main
artery that carries oxygen-rich blood to the body. The buildup of plaque inside
an artery is called
atherosclerosis
(ath-er-o-skler-O-sis).
Age-Related Changes
Men older than 65 and women older than 75 are prone
to developing calcium and other deposits on their heart valves. These deposits
stiffen and thicken the valve flaps and limit blood flow (stenosis).
The aortic valve is especially prone to this
problem. The deposits resemble those seen in the narrowed and hardened blood
vessels of people who have atherosclerosis. Some of the same processes may
cause both atherosclerosis and heart valve disease.
Rheumatic Fever
Some people have heart valve disease due to
untreated strep throat or other infections with strep bacteria, which progress
to rheumatic fever.
When the body tries to fight the strep infection,
one or more heart valves may be damaged or scarred in the process. The aortic
and mitral valves are most often affected. Symptoms due to heart valve damage
often don't appear until many years after recovery from rheumatic fever.
Today, most people with strep infections are treated
with antibiotics before rheumatic fever develops. It's very important to take
the entire amount of antibiotics your doctor prescribes for strep throat, even
if you feel better.
Heart valve disease due to rheumatic fever mainly
affects older people who had strep infections before antibiotics were
available. It also affects people from developing countries, where rheumatic
fever is more common.
Infections
Common germs that enter through the bloodstream and
get carried to the heart can sometimes infect the inner surface of the heart,
including the heart valves. This rare, but sometimes life-threatening infection
is called
endocarditis (EN-do-kar-DI-tis).
The germs can enter the bloodstream through needles,
syringes, or other medical devices and through breaks in the skin or gums.
Usually the body's defenses fight off the germs and no infection occurs.
Sometimes these defenses fail, which leads to endocarditis.
Endocarditis can develop in people who already have
abnormal blood flow through a heart valve due to congenital or acquired heart
valve disease. The abnormal blood flow causes blood clots to form on the
surface of the valve. The blood clots make it easier for germs to attach to and
infect the valve.
Endocarditis can worsen existing heart valve
disease.
Other Conditions and Factors Linked To Heart Valve
Disease
A number of other conditions and factors are
sometimes linked to heart valve disease. However, it's often unknown how these
conditions actually cause heart valve disease.
- Systemic lupus erythmatosis (SLE). SLE and other
immune diseases can affect the aortic and mitral valves.
- Carcinoid syndrome. Tumors in the digestive tract
that spread to the liver or lymph nodes can affect the tricuspid and pulmonary
valves.
- Metabolic disorders. Relatively uncommon
diseases, such as Fabry disease and hyperlipidemia, can affect the heart
valves.
- Diet medicines. The use of fenfluramine and
phentermine ("fen-phen") has sometimes been linked to heart valve problems.
These problems typically stabilize or improve after the medicine is stopped.
- Radiation therapy. Radiation therapy to the chest
area can cause heart valve disease. This therapy is used to treat cancer. Heart
valve disease due to radiation therapy may not cause symptoms for as many as 20
years after the therapy ends.
- Marfan
syndrome. Congenital disorders, such as Marfan syndrome, and other
connective tissue disorders mainly affect the structure of the body's main
arteries. However, these conditions also can also affect the heart valves.
Who Is At Risk for Heart Valve Disease?
Populations Affected
Older people are more likely to develop heart valve
disease. It's estimated that 1 in 8 people age 75 or older have at least
moderate heart valve disease.
People who have a history of endocarditis, rheumatic
fever,
heart
attack, or
heart
failure—or previous heart valve disease—are more likely to
develop heart valve disease.
About 1 to 2 percent of people are born with an
aortic valve that has two flaps instead of three. Sometimes an aortic valve may
have three flaps, but two flaps are fused together and act as one flap. This is
called a bicuspid or bicommissural aortic valve. People who have this
congenital condition are more likely to develop aortic heart valve disease.
Major Risk Factors
The major risk factors for acquired heart valve
disease are:
What Are the Signs and Symptoms of Heart Valve
Disease?
Major Signs and Symptoms
The main sign of heart valve disease is an unusual
heart sound called a
heart
murmur. Your doctor can hear a heart murmur with a stethoscope.
However, many people have heart murmurs without
having heart valve disease or any other heart problems. Others may have heart
murmurs due to heart valve disease, but have no other signs or symptoms.
Heart valve disease often worsens over time, so
signs and symptoms may develop years after a heart murmur is first heard. Many
people who have heart valve disease don't have any symptoms until they're
middle-aged or older.
Other common signs and symptoms of heart valve
disease relate to
heart
failure, which heart valve disease can eventually cause. These symptoms
include:
- Unusual fatigue (tiredness)
- Shortness of breath, especially when you exert
yourself or when you're lying down
- Swelling of your ankles, feet, or sometimes the
abdomen
Other Signs and Symptoms
Heart valve disease can cause chest pain that may
only happen when you exert yourself. You also may notice a fluttering, racing,
or irregular heartbeat. Some types of heart valve disease, such as aortic or
mitral valve stenosis, can cause dizziness or fainting.
How Is Heart Valve Disease Diagnosed?
Your primary care provider may detect a
heart
murmur or other signs of heart valve disease. However, a cardiologist will
usually diagnose the condition. A cardiologist is a doctor who specializes in
treating heart problems.
To diagnose heart valve disease, your doctor will
ask about your symptoms. (See "What Are the
Signs and Symptoms of Heart Valve Disease?")
He or she also will do a physical exam and look at
the results of medical tests and imaging.
Physical Exam
Your doctor will listen to your heart with a
stethoscope to find out if you have a heart murmur that's likely caused by a
heart valve problem.
Your doctor also will listen to your lungs as you
breathe to check for fluid buildup. He or she will check for swollen ankles and
other signs that your body is keeping in water.
Tests and Procedures
The main test for diagnosing heart valve disease is
echocardiography.
But an EKG
(electrocardiogram) or chest x ray is commonly used to reveal certain signs of
the condition. If these signs are present, echocardiography usually is done to
confirm the diagnosis.
Your doctor also may have you undergo other tests,
such as
cardiac
catheterization,
stress
testing, or
cardiac
MRI (magnetic resonance imaging), if you're diagnosed with heart valve
disease. These tests and procedures can help your doctor better assess how
severe your condition is and plan treatment.
Electrocardiogram
This is a simple test that detects and records the
electrical activity of your heart. It can detect an irregular heartbeat and
signs of a previous
heart
attack. It can also show whether certain chambers of your heart are
enlarged.
An EKG usually is done in your doctor's office.
Chest X Ray
This test can show whether certain sections of your
heart are enlarged, whether you have fluid in your lungs, or whether there are
calcium deposits in your heart.
This test helps your doctor learn which type of
valve defect you have, how severe it is, and whether you have any other heart
problems.
Echocardiography
The test uses sound waves to create a moving picture
of your heart as it beats. A wand that's placed on the surface of your chest
transmits the sound waves. Echoes from the sound waves are converted into
pictures of your heart on a computer screen.
An echocardiogram can show:
- The size and shape of your heart valves and
chambers
- How well your heart is pumping blood
- Whether a valve is narrowed or has backflow
Your doctor may recommend a transesophageal
(tranz-ih-sof-uh-JEE-ul) echocardiogram, or TEE, to get a better image.
For a TEE, the sound wave wand is put on the end of
a special tube. The tube is passed down your throat and into your esophagus
(the tube leading from your mouth to your stomach). You will be given medicine
to relax you during this procedure.
Cardiac Catheterization
For this procedure, a long, thin, flexible tube
called a catheter is put into a blood vessel in your arm, upper thigh (groin),
or neck and threaded into your heart. Your doctor uses x-ray images to guide
the catheter.
Through the catheter, your doctor does diagnostic
tests and imaging that show whether backflow is occurring through a valve and
how fully the valve opens. You're given medicine to help you relax, but you're
awake during the procedure.
Your doctor may order a cardiac catheterization if
your signs and symptoms of heart valve disease aren't in line with your
echocardiography results. The procedure also can help your doctor assess
whether your symptoms are due to specific valve problems or
coronary
artery disease. All of this information helps your doctor decide the best
way to treat you.
Stress Test
During stress testing, you exercise to make your
heart work hard and beat fast while heart tests and imaging are done. If you
can't exercise, you'll be given medicine to make your heart work hard and beat
fast.
A stress test can show whether you have signs and
symptoms of heart valve disease when your heart is working hard. It can help
your doctor assess the severity of your heart valve disease.
Cardiac MRI
Cardiac MRI uses a powerful magnet and radio waves
to make detailed images of your heart. A cardiac MRI image can confirm
information about valve defects or provide more detailed information.
This information can help your doctor plan your
treatment. An MRI also may be done before heart valve surgery to help your
surgeon plan for the surgery.
How Is Heart Valve Disease Treated?
The goals of heart valve disease treatment are
to:
- Prevent, treat, or relieve the symptoms of other
related heart conditions.
- Protect your valve from further damage.
- Repair or replace faulty valves when they cause
severe symptoms or become life threatening. Man-made or biological valves are
used as replacements.
Currently, no medicines can cure heart valve
disease. However, lifestyle changes and medicines often can successfully treat
symptoms and delay complications for many years. Eventually, though, you may
need surgery to repair or replace a faulty heart valve.
Prevent, Treat, or Relieve the Symptoms of Other
Related Heart Conditions
To relieve the symptoms of heart conditions related
to heart valve disease, your doctor may ask you to quit smoking and follow a
healthy eating plan low in salt, cholesterol, and fat.
Examples of healthy eating plans are the National
Heart, Lung, and Blood Institute's
Therapeutic
Lifestyle Changes (TLC) and
Dietary
Approaches to Stop Hypertension (DASH) eating plans. TLC is for people who
have high
blood cholesterol. DASH is for people who have
high
blood pressure (or for anyone who wants to follow a healthy eating
plan).
Your doctor also may ask you to limit physical
activities that make you unusually short of breath and fatigued (tired). He or
she also may ask that you limit competitive athletic activity, even if the
activity doesn't leave you unusually short of breath or fatigued.
Your doctor may prescribe medicines to help prevent
or treat other related heart conditions, such as
heart
failure, high blood pressure,
irregular
heartbeats,
coronary
artery disease (CAD), and life-threatening blood clots. Heart valve disease
can cause these conditions or worsen them.
People who have heart valve disease are commonly
prescribed medicines to:
- Treat heart failure. Heart failure medicines
widen blood vessels and rid the body of too much fluid.
- Lower blood pressure or blood cholesterol
levels.
- Prevent irregular heartbeats.
- Thin the blood and prevent clots (for people who
have man-made valves). These medicines also are prescribed for mitral stenosis
or other valve defects that make you prone to developing blood clots.
Protect Your Valve From Further Damage
If you've had previous heart valve disease and now
have a man-made valve, you may be at increased risk for a heart infection
called
endocarditis. This infection can worsen your heart valve
disease. Even if you don't yet have symptoms of a valve problem, you're at
increased risk for this infection.
To help prevent this serious infection, floss and
brush your teeth and see a dentist regularly. Gum infections and tooth decay
can cause endocarditis.
Let your doctors and dentists know if you have a
man-made valve or if you've had endocarditis before. They may give you
antibiotics before medical or dental procedures (such as surgery or dental
cleanings) that could allow bacteria to enter your bloodstream. Talk to your
doctor about whether you need to take antibiotics before such procedures.
Repair or Replace Heart Valves
Your doctor may recommend repairing or replacing
your heart valve(s), even if you do not yet have symptoms of heart valve
disease. This can prevent lasting damage to your heart and sudden death.
Having heart valve repair or replacement depends on
a number of factors, including:
- How severe your valve disease is.
- Your age and general health.
- Whether you need
heart
surgery for other conditions, such as
bypass
surgery to treat CAD. Bypass surgery and valve surgery can be done at the
same time.
When possible, heart valve repair is preferred over
heart valve replacement. Valve repair preserves the strength and function of
the heart muscle. People who have valve repair also have a lower risk for
endocarditis after the surgery, and they don't need to take blood-thinning
medicines for the rest of their lives.
However, heart valve repair surgery is harder to do
than valve replacement. Also, not all valves can be repaired. Mitral valves
often can be repaired. Aortic or pulmonary valves often have to be
replaced.
Repairing Heart Valves
Heart valves can be repaired by:
- Separating fused valve flaps
- Removing or reshaping tissue so the valve can
close tighter
- Adding tissue to patch holes or tears or to
increase the support at the base of the valve
Heart surgeons do most heart valve repair surgeries.
Cardiologists do some repair surgeries using
cardiac
catheterization. Although catheterization procedures are less invasive,
they also may not work as well for some patients. You and your doctor will
decide whether repair is appropriate and the best procedure for doing it.
Balloon valvuloplasty. Heart valves that
don't open fully (stenosis) can be repaired with surgery or with a less
invasive catheter procedure called balloon valvuloplasty (VAL-vyu-lo-plas-tee).
This procedure also is called balloon valvotomy.
During the procedure, a balloon-tipped tube is
threaded through your blood vessels and into the faulty valve in your heart.
The balloon is inflated to help widen the opening of the valve. Your doctor
then deflates the balloon and removes both it and the tube.
You're awake during the procedure, which usually
requires an overnight stay in the hospital.
Balloon valvuloplasty relieves many of the symptoms
of heart valve disease, but it may not cure it. The condition can still worsen
over time. You may need medicines to help with symptoms or surgery to repair or
replace the faulty valve.
Balloon valvuloplasty has a shorter recovery time
than surgery. For some patients who have mitral valve stenosis, it may work as
well as surgical repair or replacement. For these reasons, balloon
valvuloplasty usually is preferred over surgical repair or replacement for
these people. Balloon valvuloplasty doesn't work as well as surgical treatment
for adults who have aortic valve stenosis.
Balloon valvuloplasty often is used in infants and
children. In these patients, valve stenosis is caused by a congenital defect
that can be repaired by a one-time procedure.
Replacing Heart Valves
Sometimes heart valves can't be repaired and must be
replaced. This surgery involves removing the faulty valve and replacing it with
a man-made valve or a biologic valve.
Biologic valves are made from pig, cow, or human
heart tissue and may have man-made parts as well. These valves are specially
treated, so no medicines are needed to stop the body from rejecting the
valve.
Man-made valves are more durable than biologic
valves and usually don't have to be replaced. Biologic valves usually have to
be replaced after about 10 years, although newer biologic valves may last 15
years or longer.
Unlike biologic valves, however, man-made valves
require you to take blood-thinning medicines for the rest of your life. These
medicines prevent blood clots from forming on the valve. Blood clots can cause
a
heart
attack or stroke. Man-made valves also raise your risk for
endocarditis.
You and your doctor will decide together whether
you should have a man-made or biologic replacement valve. If you're a woman of
childbearing age or if you're athletic, you may prefer a biologic valve so you
don't have to take blood-thinning medicines. If you're elderly, you also may
prefer a biologic valve, as it will likely last for the rest of your life.
Other Approaches for Repairing and Replacing Heart
Valves
Some newer forms of heart valve repair or
replacement surgery are less invasive than traditional surgery. These
procedures use smaller incisions (cuts) to reach the heart valves. Hospital
stays for these newer types of surgery are usually 3 to 5 days, compared to 5
day stays for traditional heart valve surgery.
New surgeries tend to cause less pain and have a
lower risk of infection. Recovery time also tends to be shorter—2 to 4
weeks versus 6 to 8 weeks for traditional surgery.
Some cardiologists and surgeons are exploring
procedures that use
cardiac
catheterization to thread clips or other devices in a tube through your
blood vessels and into the faulty valve in your heart. The clips or devices are
used to reshape the valve and stop the backflow of blood. It's not yet known
how effective these procedures are.
The Ross operation is a surgical procedure to treat
faulty aortic valves. During this operation, your doctor removes your faulty
aortic valve and replaces it with your pulmonary valve. The pulmonary valve is
then replaced with a pulmonary valve from a deceased human donor.
This is more involved surgery than typical valve
replacement, and it has a greater risk of complications.
The Ross operation may be especially useful for
children because the surgically replaced valves continue to grow with the
child. Also, lifelong treatment with blood-thinning medicines isn't required.
But in some patients, one or both valves fail to work properly within a few
years of the surgery. Experts continue to debate the usefulness of this
procedure.
Serious risks from all types of heart valve surgery
vary according to your age, health, the type of valve defect(s) you have, and
the surgical procedure(s) performed.
How Can Heart Valve Disease Be Prevented
To prevent heart valve disease caused by rheumatic
fever, see your doctor if you have signs of a strep infection. These signs
include a red and painful sore throat, fever, and white spots on your
tonsils.
If you do have a strep infection, be sure to take
all medicines prescribed to treat it. Prompt treatment of strep infections can
prevent rheumatic fever, which damages heart valves.
It's possible that exercise, diet, and medicines
that lower cholesterol also might prevent aortic stenosis (thickening and
stiffening of the aortic valve). Researchers continue to study this
possibility.
A heart healthy eating plan, physical activity,
other lifestyle measures, or medicines aimed at preventing a
heart
attack,
high
blood pressure, or
heart
failure also might help prevent heart valve disease.
If you've had previous heart valve disease and now
have a man-made valve, you may be at higher risk for a heart infection called
endocarditis. Floss and brush your teeth regularly. Gum
infections and tooth decay can cause endocarditis.
Let your doctors and dentists know if you have a
man-made valve or if you've had endocarditis before. They may give you
antibiotics before medical or dental procedures (such as surgery or dental
cleanings) that could allow bacteria to enter your bloodstream. Talk to your
doctor about whether you need to take antibiotics before such
procedures.
Living With Heart Valve Disease
Heart valve disease is a lifelong condition.
However, many people with the condition don't have any symptoms until they're
middle-aged or older. Over time, heart valve disease may worsen and can cause
heart
failure or other life-threatening conditions.
Eventually, you may need your faulty heart valve(s)
repaired or replaced. After repair or replacement, you will still need certain
medicines and regular checkups with your doctor.
Ongoing Health Care Needs
- See your doctor regularly for checkups and for
echocardiography
or other tests. This will allow your doctor to check the progress of your heart
valve disease. Ask your doctor what physical activities are appropriate for
you.
- Call your doctor if your heart valve disease
symptoms worsen or you develop new symptoms. (See "What Are the Signs and Symptoms of Heart Valve
Disease?")
- Call your doctor if you develop symptoms of
endocarditis. Symptoms of this heart infection include fever,
chills, muscle aches, night sweats, difficulty breathing, fatigue (tiredness),
weakness, red spots on the palms and soles, and swelling of the feet, legs, and
belly.
- Let your doctors and dentists know if you have a
man-made valve or if you've had endocarditis before. They may give you
antibiotics before medical or dental procedures (such as surgery or dental
cleanings) that could allow bacteria to enter your bloodstream. Talk to your
doctor about whether you need to take antibiotics before such procedures.
- Take all your prescribed medicines.
Pregnancy and Heart Valve Disease
Mild to moderate heart valve disease during
pregnancy usually can be managed with medicines or bed rest without posing
heightened risks to the mother or fetus.
Most heart valve conditions can be treated with
medicines that are safe to take during pregnancy. Your doctor can advise you on
which medicines are safe for you.
Severe heart valve disease can make pregnancy or
labor and delivery riskier. If you have severe heart valve disease and/or its
symptoms, consider having your heart valves repaired or replaced before getting
pregnant. Such repair or replacement also can be done during pregnancy, if
needed. But this surgery poses danger to both the mother and fetus.
Key Points
- Heart valve disease is a condition in which one
or more of your heart valves don't work properly. The heart has four valves:
the tricuspid, pulmonary, mitral, and aortic valves.
- These valves have tissue flaps that open and
close with each heartbeat. These flaps make sure blood flows in the right
direction through your heart's four chambers and to the rest of your body.
- Heart valves can have three basic kinds of
problems:
- Regurgitation, or backflow, occurs when a
valve doesn't close tightly. Blood leaks back into the heart chamber rather
than flowing forward through the heart or into an artery.
- Stenosis occurs when the flaps of a valve
thicken, stiffen, or fuse together. This prevents the heart valve from fully
opening, and not enough blood flows through the valve.
- Atresia occurs when a valve lacks an opening
for blood to pass through.
- Heart valve disease can make your heart work
harder and affect its ability to pump blood. If not treated, advanced heart
valve disease can cause
heart
failure, stroke, blood clots, or sudden death due to
sudden
cardiac arrest.
- You can be born with heart valve disease or
develop it later in life. It's not known what causes the type of valve disease
that people are born with. Heart conditions and other disorders, age-related
changes, rheumatic fever, and infections can cause heart valve disease that
develops later in life.
- The major risk factors for acquired heart valve
disease are age, having risk factors for heart disease, and having risk factors
for the heart infection
endocarditis.
- Many people don't have signs or symptoms of heart
valve disease until they're middle-aged or older.
- The main sign of heart valve disease is a
heart
murmur (an unusual heart sound). Other common signs and symptoms are
unusual fatigue (tiredness), shortness of breath, and swelling of your ankles,
feet, or abdomen.
- Heart valve disease is diagnosed based on your
symptoms, a physical exam, and the results from tests and procedures.
- Currently, no medicines can cure heart valve
disease. However, lifestyle changes and medicines often can successfully treat
symptoms and delay complications for many years. Eventually, you may need to
have your faulty valve repaired or replaced with a man-made or biological
valve.
- When possible, heart valve repair is preferred
over heart valve replacement. Valve repair preserves the strength and function
of the heart muscle. People who have valve repair also have a lower risk for
endocarditis after the surgery, and they don't need to take blood-thinning
medicines for the rest of their lives.
- To prevent heart valve disease caused by
rheumatic fever, see your doctor if you have signs of a strep infection. This
infection can cause rheumatic fever, which can damage the heart valves. If you
do have a strep infection, take all medicines as prescribed.
- Heart valve disease is a lifelong condition. If
you have the condition, it's important to have ongoing medical care. See your
doctor regularly. Call your doctor if your signs or symptoms worsen or if you
have signs or symptoms of endocarditis. Take all your medicines as
prescribed.
- Mild to moderate heart valve disease during
pregnancy usually can be managed with medicines or bed rest without posing
heightened risks to the mother or fetus. Your doctor can advise you on which
medicines are appropriate during pregnancy.
- Severe heart valve disease can make pregnancy or
labor and delivery riskier. If you have severe valve disease and/or its
symptoms, consider having your heart valves repaired or replaced before getting
pregnant. Such repair or replacement also can be done during pregnancy, if
needed. But this surgery poses danger to both the mother and fetus.
Links to Other Information About Heart Valve
Disease
NHLBI Resources
Non-NHLBI Resources
Clinical Trials
|

