What Is Pneumonia?
Pneumonia (nu-MO-ne-ah) is an infection in one or
both of the lungs. Many small germs, such as bacteria, viruses, and fungi, can
cause pneumonia.
The infection causes your lungs’ air sacs,
called alveoli (al-VEE-uhl-eye), to become inflamed. The air sacs may fill up
with fluid or pus, causing symptoms such as a cough (with phlegm), fever,
chills, and trouble breathing.
Overview
Pneumonia and its symptoms can vary from mild to
severe. Many factors affect how serious pneumonia is, such as the type of germ
causing the infection and your age and overall health.
Pneumonia tends to be more serious for:
- Infants and young children.
- Older adults (people 65 years or older).
- People who have other health problems like
heart
failure,
diabetes, or
COPD
(chronic obstructive pulmonary disease).
- People who have weak immune systems as a result
of diseases or other factors. These may include HIV/AIDS, chemotherapy (a
treatment for cancer), or an organ or
bone
marrow transplant.
Outlook
Pneumonia is common in the United States. Treatment
for pneumonia depends on its cause, how severe your symptoms are, and your age
and overall health. Many people can be treated at home, often with oral
antibiotics.
Children usually start to feel better in 1 to 2
days. For adults, it usually takes 2 to 3 days. Anyone whose symptoms get worse
should be checked by a doctor.
People who have more severe symptoms or underlying
health problems may need treatment in a hospital. It may take 3 weeks or more
before they can go back to their normal routines.
Fatigue (tiredness) from pneumonia can last for a
month or more.
Types of Pneumonia
Pneumonia is named for the way in which a person
gets the infection or for the germ that causes it.
Community-Acquired Pneumonia
Community-acquired pneumonia (CAP) occurs outside of
hospitals and other health care settings. Most people get CAP by breathing in
germs (especially while sleeping) that live in the mouth, nose, or throat.
CAP is the most common type of pneumonia. Most cases
occur during the winter. About 4 million people get this form of pneumonia each
year. About 1 out of every 5 people who has CAP needs to be treated in a
hospital.
Hospital-Acquired Pneumonia
Some people catch pneumonia during a hospital stay
for another illness. This is called hospital-acquired pneumonia (HAP).
You’re at higher risk for getting HAP if you’re on a mechanical
ventilator (a machine that helps you breathe).
HAP tends to be more serious than CAP. This is
because you’re already sick. Also, hospitals tend to have more germs that
are resistant to antibiotics—a treatment for pneumonia.
Health Care-Associated Pneumonia
Patients also may get pneumonia in other health care
settings, such as nursing homes, dialysis centers, and outpatient clinics. This
is called health care-associated pneumonia.
Other Common Types of Pneumonia
Aspiration Pneumonia
This type of pneumonia occurs when you accidentally
inhale food, drink, vomit, or saliva from your mouth into your lungs. This
usually happens when something disturbs your normal gag reflex, such as a brain
injury, swallowing problem, or excessive use of alcohol or drugs.
Aspiration pneumonia can cause pus to form in a
cavity in the lung. This is called a lung abscess.
Atypical Pneumonia
Several types of bacteria—Legionella
pneumophila, mycoplasma pneumonia, and Chlamydophila
pneumoniae—cause this type of CAP. Atypical pneumonia is passed from
person to person.
Other Names for Pneumonia
- Pneumonitis (nu-mo-NI-tis).
- Bronchopneumonia (BRONG-ko-nu-MO-ne-ah).
- Nosocomial (nos-o-KO-me-al) pneumonia. This is
another name for hospital-acquired pneumonia.
- Walking pneumonia. This refers to pneumonia
that’s mild enough that you’re not bedridden.
- Double pneumonia. This refers to pneumonia that
affects both lobes of the lungs.
What Causes Pneumonia?
Many different germs can cause pneumonia. These
include different kinds of bacteria, viruses, and, less often, fungi.
Most of the time, the body filters germs out of the
air that we breathe to protect the lungs from infection. (For more information,
see the Diseases and Conditions Index
“How
the Lungs Work” article.) Sometimes, though, germs manage to enter
the lungs and cause infections. This is more likely to occur when:
- Your immune system is weak
- A germ is very strong
- Your body fails to filter germs out of the air
that you breathe
Your mouth and airways are exposed to germs as you
inhale air through your nose and mouth. Your immune system, the shape of your
nose and throat, your ability to cough, and fine, hair-like structures called
cilia (SIL-e-ah) help stop the germs from reaching your lungs.
For example, coughing is one way the body keeps
germs from reaching the lungs. Some people may not be able to cough because,
for example, they’ve had a stroke or are sedated (given medicine to make
them sleepy). This means germs may remain in the airways rather than being
coughed out.
When germs do reach your lungs, your immune system
goes into action. It sends many kinds of cells to attack the germs. These cells
cause the alveoli (air sacs) to become red and inflamed and to fill up with
fluid and pus. This causes the symptoms of pneumonia.
Germs That Can Cause Pneumonia
Bacteria
Bacteria are the most common cause of pneumonia in
adults. Some people, especially the elderly and those who are disabled, may get
bacterial pneumonia after having the flu or even a common cold.
Dozens of different types of bacteria can cause
pneumonia. Bacterial pneumonia can occur on its own or develop after you've had
a cold or the flu. This type of pneumonia often affects one lobe, or area, of a
lung. When this happens, the condition is called lobar pneumonia.
The most common cause of pneumonia in the United
States is the bacterium Streptococcus (strep-to-KOK-us)
pneumoniae, or pneumococcus (nu-mo-KOK-us).
Lobar Pneumonia
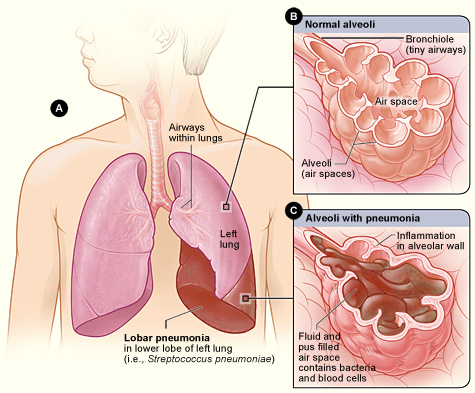
Figure A shows the location of the
lungs and airways in the body. It also shows pneumonia that’s affecting
the lower lobe of the left lung. Figure B shows normal alveoli. Figure C shows
infected alveoli.
Another type of bacterial pneumonia is called
atypical pneumonia. Atypical pneumonia includes:
- Legionella pneumophila. This is
sometimes called Legionnaire's disease. This type of pneumonia has caused
serious outbreaks. Outbreaks have been linked to exposure to cooling towers,
whirlpool spas, and decorative fountains.
- Mycoplasma pneumonia. This is
a common type of pneumonia that usually affects people younger than 40. People
who live or work in crowded places like schools, homeless shelters, and prisons
are most likely to get it. It’s usually mild and responds well to
treatment with antibiotics. But, it can be very serious in some people. It may
be associated with a skin rash and hemolysis (the breakdown of red blood
cells).
- Chlamydophila pneumoniae. This kind of
pneumonia can occur all year and is often mild. The infection is most common in
people 65 to 79 years of age.
Viruses
Respiratory viruses cause up to one-third of the
pneumonia cases in the United States each year. These viruses are the most
common cause of pneumonia in children younger than 5 years.
Most cases of viral pneumonia are mild. They get
better in about 1 to 3 weeks without treatment. Some cases are more serious and
may require treatment in a hospital.
If you have viral pneumonia, you run the risk of
getting bacterial pneumonia also.
The flu virus is the most common cause of viral
pneumonia in adults. Other viruses that cause pneumonia include respiratory
syncytial virus, rhinovirus, herpes simplex virus, severe acute respiratory
syndrome (SARS), and more.
Fungi
Three types of fungi in the soil in some parts of
the United States can cause pneumonia. These fungi are coccidioidomycosis
(kok-sid-e-OY-do-mi-KO-sis) in Southern California and the desert Southwest,
histoplasmosis (HIS-to-plaz-MO-sis) in the Ohio and Mississippi River Valleys,
and cryptococcus (krip-to-KOK-us). Most people exposed to these fungi
don’t get sick, but some do and require treatment.
Serious fungal infections are most common in people
who have weak immune systems as a result of long-term use of medicines to
suppress their immune systems or having HIV/AIDS.
Pneumocystis jirovecii (nu-mo-SIS-tis ye-RO-VECH-e),
formerly Pneumocystis carinii, is sometimes considered a fungal pneumonia.
However, it’s not treated with the usual antifungal medicines. It usually
affects people who:
- Have HIV/AIDS or cancer
- Have had an organ and/or
bone
marrow transplant
- Take medicines that affect their immune systems
Other kinds of fungal infections also can lead to
pneumonia.
Who Is At Risk for Pneumonia?
Pneumonia can affect people of all ages. However,
two age groups are at greater risk of developing pneumonia:
- Infants who are 2 years or younger, because their
immune systems are still developing during the first few years of life
- People who are 65 years or older
Other conditions and factors also raise your risk
for pneumonia. You’re more likely to get pneumonia if you have a lung
disease or other serious disease. Examples include
cystic
fibrosis,
asthma,
COPD
(chronic obstructive pulmonary disease),
bronchiectasis,
diabetes,
heart
failure, and
sickle
cell anemia.
You’re at greater risk for pneumonia if
you’re in a hospital intensive-care unit, especially if you’re on a
ventilator (a machine to help you breathe).
Having a weak or suppressed immune system also can
raise your risk. A weak immune system may be the result of a disease such as
HIV/AIDS. A suppressed immune system may be due to an organ or
bone
marrow transplant, chemotherapy (treatment for cancer), or long-term
steroid use.
Your risk also goes up if you have trouble coughing
because of a stroke, trouble swallowing, limited ability to move, alcohol use,
or sedation (being given medicine to make you relaxed or sleepy).
Smoking cigarettes, abusing alcohol, and being
undernourished also raise your risk for pneumonia. Your risk also goes up if
you’ve recently had a cold or the flu, or if you’re exposed to
certain chemicals, pollutants, or toxic fumes.
What Are the Signs and Symptoms of Pneumonia?
The symptoms of pneumonia vary from mild to severe.
Many factors affect how serious pneumonia is, including the type of germ
causing the infection and your age and overall health. (For more information,
see “Who Is At Risk for
Pneumonia?” )
See your doctor promptly if you:
- Have a high fever
- Have shaking chills
- Have a cough with phlegm, which doesn’t
improve or worsens
- Develop shortness of breath with normal daily
activities
- Have chest pain when you breathe or cough
- Feel suddenly worse after a cold or the flu
People with pneumonia may have other symptoms,
including nausea (feeling sick to your stomach), vomiting, and diarrhea.
Symptoms may vary in certain populations. Newborns
and infants may not show any signs of the infection or may vomit, have a fever
and cough, or appear restless, sick, or tired and without energy.
Older adults and people who have serious illnesses
or weak immune systems may have fewer and milder symptoms. They may even have a
lower than normal temperature. If they already have a lung disease, it may get
worse. Older adults who have pneumonia sometimes have sudden changes in mental
awareness.
Complications of Pneumonia
Often, people who have pneumonia can be treated
successfully and not have complications. But some patients, especially those in
high-risk groups, may have complications such as:
- Bacteremia (bak-ter-E-me-ah). This serious
complication occurs when the infection moves into your bloodstream. From there,
it can quickly spread to other organs, including your brain.
- Lung abscess. An abscess occurs when pus forms in
a cavity in the lung. An abscess usually is treated with antibiotics. In some
cases, surgery or needle drainage is needed to remove it.
-
Pleural effusion. Pneumonia may cause fluid to build up in the pleural
space, which is the space between your lungs and chest wall. Pneumonia can
cause the fluid to become infected—a condition called empyema
(em-pi-E-ma). If this happens, you may need to have the fluid drained through a
chest tube or removed through surgery.
How Is Pneumonia Diagnosed?
Pneumonia can be hard to diagnose because it may
seem like a cold or the flu. People may not realize it’s more serious
until it lasts longer than these other conditions.
Your doctor will diagnose pneumonia based on your
medical history and the results from a physical exam and tests.
Medical History
Your doctor will ask about your
signs and symptoms and how and when
they began. To find out what type of germ is causing the pneumonia, he or she
also may ask about:
- Any recent traveling you’ve done
- Your hobbies
- Your exposure to animals
- Your exposure to sick people at home, school, or
work
- Your past and current medical conditions, and
whether any have gotten worse recently
- Any medicines you take
- Whether you smoke
- Whether you've had a flu or pneumonia vaccination
Physical Exam
Your doctor will listen to your lungs with a
stethoscope. If you have pneumonia, your lungs may make crackling, bubbling,
and rumbling sounds when you inhale. It may be hard to hear sounds of breathing
in some areas of your chest. Your doctor also may hear wheezing.
Diagnostic Tests
If your doctor suspects you have pneumonia, he or
she also may order one or more of the following tests.
Chest X Ray
A
chest
x ray is a painless test that creates pictures of the structures inside
your chest, such as your heart and lungs.
A chest x ray is the best test for diagnosing
pneumonia. However, this test won’t tell your doctor what kind of germ is
causing the pneumonia.
Blood Tests
Blood
tests involve taking a sample of blood from a vein in your body. A complete
blood count (CBC) measures many parts of your blood, including the number of
white blood cells in the blood sample. The number of white blood cells can show
whether you have a bacterial infection.
Your doctor also may order a blood culture to find
out whether the infection has spread to your bloodstream. This test is used to
detect germs in the bloodstream. It may show which germ caused the infection.
If so, your doctor can decide how to treat the infection.
Other Tests
You may need other tests if you’re in the
hospital, have serious symptoms, are older, or have other health problems.
Sputum test. Your doctor may look
at a sample of sputum (spit) collected from you after a deep cough. This may
help your doctor find out what germ is causing your pneumonia . Then, he or she
can plan treatment.
Chest CT scan. A
chest CT scan is a painless test that
creates precise pictures of the structures in your chest, such as your lungs. A
chest CT scan is a kind of x ray, but its pictures show more detail than those
of a standard chest x ray.
Pleural fluid culture. For this
test, a sample of fluid is taken from the space between your lungs and chest
wall (the pleural space). This is done using a procedure called
thoracentesis
(THOR-a-sen-TE-sis). The fluid is studied for germs that may cause pneumonia.
Pulse oximetry. For this test, a
small clip is attached to your finger or ear to show how much oxygen is in your
blood. Pneumonia can keep your lungs from moving enough oxygen into your
bloodstream.
If you’re very sick, your doctor may need to
measure the level of oxygen in your blood using a blood sample. The sample is
taken from an artery, usually in your wrist.
Bronchoscopy.
Bronchoscopy
(bron-KOS-ko-pee) is a procedure used to look inside the lungs' airways. If
you’re in the hospital and treatment with antibiotics isn’t working
well, your doctor may use this test.
Your doctor passes a thin, flexible tube with a
camera on its tip through your nose or mouth, down your throat, and into the
airways.
This test allows your doctor to see whether
something is blocking your airways or whether another factor is contributing to
your pneumonia.
How Is Pneumonia Treated?
Treatment for pneumonia depends on the type of
pneumonia you have and how severe it is. Most people who have
community-acquired pneumonia—the most common type of pneumonia—are
treated at home.
The goals of treatment are to cure the infection and
prevent complications.
General Treatment
It’s important to follow your treatment plan,
take all medicines as prescribed, and get ongoing medical care. Talk to your
doctor about when you should schedule followup care. Your doctor may want you
to have a
chest
x ray to make sure the pneumonia is gone.
Although you may start feeling better after a few
days or weeks, fatigue (tiredness) can persist for up to a month or more.
People who are treated in the hospital may need at least 3 weeks before they
can go back to their normal routines.
Bacterial Pneumonia
Bacterial pneumonia is treated with antibiotics. You
should take antibiotics as your doctor prescribes. You may start to feel better
before you finish the medicine, but you should continue taking it as
prescribed. If you stop too soon, the pneumonia may come back.
Most people begin to improve after 1 to 3 days of
antibiotic treatment. This means that they should feel better and have fewer
symptoms, such as cough and fever.
Viral Pneumonia
Viral pneumonia isn’t treated with
antibiotics. This type of medicine doesn’t work when a virus causes the
pneumonia. If you have viral pneumonia, your doctor may prescribe an antiviral
medicine to treat it.
Viral pneumonia usually improves in 1 to 3 weeks.
Treating Severe Symptoms
You may need to be treated in a hospital if:
- Your symptoms are severe
- You’re at risk for complications because of
other health problems.
If the level of oxygen in your bloodstream is low,
you may receive oxygen. If you have bacterial pneumonia, your doctor may give
you antibiotics through an intravenous (IV) line inserted into a vein.
How Can Pneumonia Be Prevented?
Pneumonia can be very serious and even life
threatening. When possible, take steps to prevent the infection, especially if
you’re in a high-risk group.
Vaccines
Vaccines are available to prevent pneumococcal
pneumonia and the flu. Vaccines can’t prevent all cases of infection.
However, compared to people who don’t get vaccinated, those who do and
still get pneumonia tend to have:
- Milder cases of the infection
- Pneumonia that doesn’t last as long
- Fewer serious complications
Pneumococcal Pneumonia Vaccine
A vaccine is available to prevent pneumococcal
pneumonia. In most people, one shot is good for at least 5 years of protection.
This vaccine is often recommended for:
- People who are 65 years or older.
- People who have chronic diseases, serious
long-term health problems, or weak immune systems. Examples include people who
have cancer, HIV/AIDS, or damaged or removed spleens.
- Alaska Natives and certain American Indian
populations.
- Children who are 2 years or younger, and children
between the ages of 2 and 5 who have a chronic disease (like cancer or
HIV/AIDS) or are Alaska Natives, American Indians, or African Americans. The
vaccine also is recommended for children between the ages of 2 and 5 who attend
group daycare programs.
Influenza Vaccine
The vaccine that helps prevent the flu is good for 1
year. It’s usually given in October or November, before peak flu season.
Because many people get pneumonia after having the
flu, this vaccine also helps prevent pneumonia.
Hib Vaccine
Haemophilus influenzae type b (Hib) is a
type of bacteria that can cause pneumonia and meningitis (an infection of the
covering of the brain and spinal cord). The Hib vaccine is given to children to
help prevent these infections.
The vaccine is recommended for all children in the
United States who are younger than 5 years. It’s often given to infants
starting at 2 months of age.
Other Ways To Help Prevent Pneumonia
Other steps also can help prevent pneumonia.
- Wash your hands with soap and water or
alcohol-based rubs to kill germs.
- Don’t smoke. Smoking damages your
lungs’ ability to filter out and defend against germs.
- Keep your immune system strong. Get plenty of
rest and physical activity and follow a healthy diet.
If you have pneumonia, limit contact with family and
friends. Cover your nose and mouth while coughing or sneezing, and dispose of
tissues right away. These measures help keep the infection from
spreading.
Living With Pneumonia
If you have pneumonia, you can take steps to recover
from the infection and prevent complications.
- Get plenty of rest.
- Follow the treatment plan your doctor gives
you.
- Take all medicines as your doctor prescribes. If
you’re using antibiotics, continue to take the medicine until it’s
all gone. You may start to feel better before you finish the medicine, but you
should continue to take it. If you stop too soon, the pneumonia may come
back.
- Talk to your doctor about when to schedule
followup care. Your doctor may order a
chest
x ray to make sure the infection is gone.
It may take time to recover from pneumonia. Some
people feel better and are able to return to their normal routines within a
week. For other people, it can take a month or more. Most people continue to
feel tired for about a month. Talk to your doctor about when you can go back to
your normal activities.
Key Points
- Pneumonia is an infection in one or both of your
lungs. Many small germs, such as bacteria, viruses, and fungi, can cause
pneumonia.
- The infection causes your lungs’ air sacs,
called alveoli, to become inflamed. The air sacs may fill up with fluid or pus,
causing symptoms such as a cough (with phlegm), fever, chills, and trouble
breathing.
- Pneumonia and its symptoms can vary from mild to
severe. Many factors affect how serious pneumonia is, including the type of
germ causing the infection and your age and overall health.
- Pneumonia tends to be more serious for infants
and young children, older adults (people 65 years or older), people who have
other chronic health problems, and people who have weak immune systems as a
result of diseases or other factors.
- Your doctor will diagnose pneumonia based on your
medical history and the results from a physical exam and tests.
- Treatment for pneumonia depends on its cause, how
severe your symptoms are, and your age and overall health. The goals of
treatment are to cure the infection and prevent complications. People who have
more severe symptoms or underlying health problems may need treatment in the
hospital.
- Pneumonia can be very serious and even life
threatening. When possible, take steps to prevent the infection. Vaccines are
available to prevent pneumococcal pneumonia and the flu. Other steps also can
help prevent pneumonia:
- Wash your hands with soap and water or
alcohol-based rubs to kill germs.
- Don’t smoke. Smoking damages your
lungs’ ability to filter out and defend against germs.
- Keep your immune system strong. Get plenty of
rest and physical activity and follow a healthy diet.
- If you have pneumonia, limit contact with family
and friends. Cover your nose and mouth while coughing or sneezing, and dispose
of tissues right away. Follow the treatment plan your doctor gives you and get
plenty of rest.
- It may take time to recover from pneumonia. Some
people feel better and are able to return to their normal routines within a
week. For other people, it can take a month or more. Talk to your doctor about
when you can go back to your normal routine.
Links to Other Information About Pneumonia
NHLBI Resources
Non-NHLBI Resources
Clinical Trials
|

