|
|
|||||
|
|
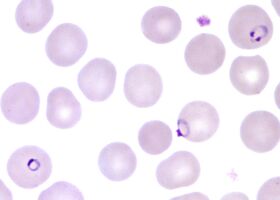
A 49-year-old man from Pennsylvania receives 4 units of packed red blood cells (PRBCs) on January 15 while undergoing hip replacement surgery. He is again hospitalized on February 1 with fever, hypotension, and renal failure. Peripheral blood smears show malaria infection. The patient has never traveled outside the United States. All patients were infected by the same parasite species shown in the figure. 1. What is that species? The patient is treated with intravenous quinidine and doxycycline and exchange transfusion.2. Among the modes of infection below, which one(s) need to be given the most serious consideration?
3. What are the next steps of this epidemiologic investigation to determine the mode of transmission?
Stored serum samples from all donors are tested. One donor has elevated IFA titers (1:16,384 to P. falciparum, 1:16,384 to P. malariae, 1:1024 to P. ovale, and 1:256 to P. vivax) indicating previous malaria infection. Though microscopy is negative, PCR performed on a stored sample from this same donor from the time of donation detects P. falciparum, indicating active infection . This donor was born in west Africa, had lived in Europe, then returned to west Africa where he had lived for approximately 20 years before immigrating to the United States 2 years ago. Donors who have been implicated as infection sources in transfusion-transmitted malaria cases often have had undetectable levels of parasitemia; therefore, antibody detection has been the method of choice to identify infected donors in CDC investigations of transfusion-transmitted malaria cases. Malaria antibody testing is 95% sensitive and 99% specific. Because the donor emigrated from an area with endemic malaria, the predictive value positive for this test is high. No available laboratory test is suitable for screening donated blood for malaria. Such a test would require 1) large-scale use design, 2) high sensitivity and specificity, and 3) ability to detect all four species of Plasmodium that affect humans. In the United States , prevention of transfusion-transmitted malaria largely depends on careful questioning of prospective donors to defer those at increased risk for malaria. The Food and Drug Administration (FDA) recommends deferring residents of malaria-endemic areas for 3 years after they emigrate from those areas and deferring persons who have had malaria for 3 years after they become asymptomatic; the American Association of Blood Banks has published standards consistent with FDA recommendations (Box).
In this case, the donor from west Africa should have been deferred. The case described in this report underscores the importance of close cooperation between managers of blood collection centers and state and federal public health officials whenever transfusion-related illness occurs. Such cooperation can facilitate traceback investigations and ensure prompt care of both donors and recipients, helping to strengthen the screening process, making blood transfusion as safe as possible, and ensuring an adequate supply of a lifesaving resource. Key Points
Selected references related to transfusion-transmitted malariaTransfusion-transmitted malaria-- Missouri and Pennsylvania, 1996-1998. MMWR Morb Mortal Wkly Rep 1999; 48: 253-6. Mungai M, Tegtmeier G, Chamberland M, Parise M. Transfusion-transmitted malaria in the United States from 1963 through 1999. N Engl J Med 2001; 344:1973--8. Probable transfusion-transmitted malaria-- Houston, Texas, 2003. MMWR Morb Mortal Wkly Rep 2003; 52: 1075-6. Page last modified : April 23, 2004 Content source: Division of Parasitic Diseases National Center for Zoonotic, Vector-Borne, and Enteric Diseases (ZVED)
|
|
||||||||||||||||||||||
| Home | Policies and Regulations | Disclaimer | e-Government | FOIA | Contact Us | ||||||
|