What Is COPD?
Chronic obstructive pulmonary disease (COPD) is a
lung disease in which the lungs are damaged, making it hard to breathe. In
COPD, the airways—the tubes that carry air in and out of your
lungs—are partly obstructed, making it difficult to get air in and out.
Cigarette smoking is the most common cause of COPD.
Most people with COPD are smokers or former smokers. Breathing in other kinds
of lung irritants, like pollution, dust, or chemicals, over a long period of
time may also cause or contribute to COPD.
The airways branch out like an upside-down tree, and
at the end of each branch are many small, balloon-like air sacs called alveoli
(al-VEE-uhl-EYE). In healthy people, each airway is clear and open. The air
sacs are small and dainty, and both the airways and air sacs are elastic and
springy. When you breathe in, each air sac fills up with air like a small
balloon; when you breathe out, the balloon deflates and the air goes out. (See
the How the Lungs Work section for
details.) In COPD, the airways and air sacs lose their shape and become floppy.
Less air gets in and less air goes out because:
- The airways and air sacs lose their elasticity
(like an old rubber band).
- The walls between many of the air sacs are
destroyed.
- The walls of the airways become thick and
inflamed (swollen).
- Cells in the airways make more mucus (sputum)
than usual, which tends to clog the airways.
COPD
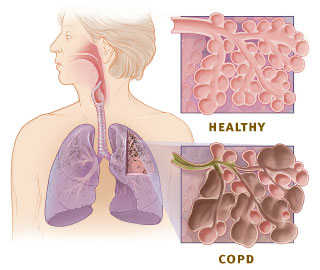
The illustration show the
respiratory system and cross-sections of healthy alveoli and alveoli with
COPD.
COPD develops slowly, and it may be many years
before you notice symptoms like feeling short of breath. Most of the time, COPD
is diagnosed in middle-aged or older people.
COPD is a major cause of death and illness, and it
is the fourth leading cause of death in the United States and throughout the
world.
There is no cure for COPD. The damage to your
airways and lungs cannot be reversed, but there are things you can do to feel
better and slow the damage.
COPD is not contagious—you cannot catch it from
someone else.
How the Lungs Work
The lungs provide a very large surface area (the
size of a football field) for the exchange of oxygen and carbon dioxide between
the body and the environment.
A slice of normal lung looks like a pink sponge
filled with tiny bubbles or holes. These bubbles, surrounded by a fine network
of tiny blood vessels, give the lungs a large surface to exchange oxygen (into
the blood where it is carried throughout the body) and carbon dioxide (out of
the blood). This process is called gas exchange. Healthy lungs do this very
well.
Here is how normal breathing works:
- You breathe in air through your nose and mouth.
The air travels down through your windpipe (trachea) then through large and
small tubes in your lungs called bronchial (BRON-kee-ul) tubes. The larger
tubes are bronchi (BRONK-eye), and the smaller tubes are bronchioles
(BRON-kee-oles). Sometimes the word "airways" is used to refer to the various
tubes or passages that air must travel through from the nose and mouth into the
lungs. The airways in your lungs look something like an upside-down tree with
many branches.
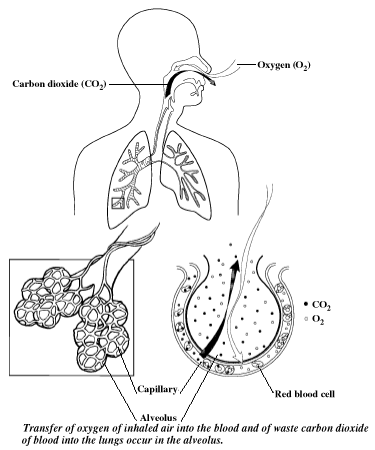
- At the ends of the small bronchial tubes, there
are groups of tiny air sacs called alveoli. The air sacs have very thin walls,
and small blood vessels called capillaries run in the walls. Oxygen passes from
the air sacs into the blood in these small blood vessels. At the same time,
carbon dioxide passes from the blood into the air sacs. Carbon dioxide, a
normal byproduct of the body's metabolism, must be removed.
The airways and air sacs in the lung are normally
elastic—that is, they try to spring back to their original shape after
being stretched or filled with air, just the way a new rubber band or balloon
would. This elastic quality helps retain the normal structure of the lung and
helps to move the air quickly in and out. In COPD, much of the elastic quality
is gone, and the airways and air sacs no longer bounce back to their original
shape. This means that the airways collapse, like a floppy hose, and the air
sacs tend to stay inflated. The floppy airways obstruct the airflow out of the
lungs, leading to an abnormal increase in the lungs' size. In addition, the
airways may become inflamed and thickened, and mucus-producing cells produce
more mucus, further contributing to the difficulty of getting air out of the
lungs.
Other Names for COPD
- Chronic obstructive airway disease
- Chronic obstructive lung disease
In the United States, chronic obstructive pulmonary
disease (COPD) includes:
- Emphysema
- Chronic bronchitis
In the emphysema type of COPD, the walls between
many of the air sacs are destroyed, leading to a few large air sacs instead of
many tiny ones (see the How the Lungs Work
section). Consequently, the lung looks like a sponge with many large bubbles or
holes in it, instead of a sponge with very tiny holes. The large air sacs have
less surface area for the exchange of oxygen and carbon dioxide than healthy
air sacs. Poor exchange of the oxygen and carbon dioxide causes shortness of
breath.
In chronic bronchitis, the airways have become
inflamed and thickened, and there is an increase in the number and size of
mucus-producing cells. This results in excessive mucus production, which in
turn contributes to cough and difficulty getting air in and out of the lungs.
Most people with COPD have both chronic bronchitis
and emphysema.
What Causes COPD?
Smoking Is the Most Common Cause of COPD
Most cases of chronic obstructive pulmonary disease
(COPD) develop after repeatedly breathing in fumes and other things that
irritate and damage the lungs and airways. Cigarette smoking is the most common
irritant that causes COPD. Pipe, cigar, and other types of tobacco smoke can
also cause COPD, especially if the smoke is inhaled. Breathing in other fumes
and dusts over a long period of time may also cause COPD. The lungs and airways
are highly sensitive to these irritants. They cause the airways to become
inflamed and narrowed, and they destroy the elastic fibers that allow the lung
to stretch and then return to its resting shape. This makes breathing air in
and out of the lungs more difficult.
Other things that may irritate the lungs and
contribute to COPD include:
- Working around certain kinds of chemicals and
breathing in the fumes for many years
- Working in a dusty area over many years
- Heavy exposure to air pollution
Being around secondhand smoke (smoke in the air from
other people smoking cigarettes) also plays a role in an individual developing
COPD.
Genes—tiny bits of information in your body
cells passed on by your parents—may play a role in developing COPD. In
rare cases, COPD is caused by a gene-related disorder called
alpha 1 antitrypsin deficiency. Alpha 1 antitrypsin
(an-te-TRIP-sin) is a protein in your blood that inactivates destructive
proteins. People with antitrypsin deficiency have low levels of alpha 1
antitrypsin; the imbalance of proteins leads to the destruction of the lungs
and COPD. If people with this condition smoke, the disease progresses more
rapidly.
Who Is At Risk for COPD?
Most people with chronic obstructive pulmonary
disease (COPD) are smokers or were smokers in the past. People with a family
history of COPD are more likely to get the disease if they smoke. The chance of
developing COPD is also greater in people who have spent many years in contact
with lung irritants, such as:
- Air pollution
- Chemical fumes, vapors, and dusts usually linked
to certain jobs
A person who has had frequent and severe lung
infections, especially during childhood, may have a greater chance of
developing lung damage that can lead to COPD. Fortunately, this is much less
common today with antibiotic treatments.
Most people with COPD are at least 40 years old or
around middle age when symptoms start. It is unusual, but possible, for people
younger than 40 years of age to have COPD.
What Are the Signs and Symptoms of COPD?
The signs and symptoms of chronic obstructive
pulmonary disease (COPD) include:
- Cough
- Sputum (mucus) production
- Shortness of breath, especially with
exercise
- Wheezing (a whistling or squeaky sound when you
breathe)
- Chest tightness
A cough that doesn't go away and coughing up lots of
mucus are common signs of COPD. These often occur years before the flow of air
in and out of the lungs is reduced. However, not everyone with a cough and
sputum production goes on to develop COPD, and not everyone with COPD has a
cough.
The severity of the symptoms depends on how much of
the lung has been destroyed. If you continue to smoke, the lung destruction is
faster than if you stop smoking.
How Is COPD Diagnosed?
Doctors consider a diagnosis of chronic obstructive
pulmonary disease (COPD) if you have the typical symptoms and a history of
exposure to lung irritants, especially cigarette smoking. A medical history,
physical exam, and breathing tests are the most important tests to determine if
you have COPD.
Your doctor will examine you and listen to your
lungs. Your doctor will also ask you questions about your family and medical
history and what lung irritants you may have been around for long periods of
time.
Breathing Tests
Your doctor will use a breathing test called
spirometry (speh-ROM-eh-tree) to confirm a diagnosis of COPD. This test is easy
and painless and shows how well your lungs work. You breathe hard into a large
hose connected to a machine called a spirometer (speh-ROM-et-er). When you
breathe out, the spirometer measures how much air your lungs can hold and how
fast you can blow air out of your lungs after taking a deep breath.
Spirometry is the most sensitive and commonly used
test of lung functions. It can detect COPD long before you have significant
symptoms.
Based on this test, your doctor can determine if you
have COPD and how severe it is. Doctors classify the severity of COPD as:
- At risk (for developing COPD). Breathing test is
normal. Mild signs that include a chronic cough and sputum production.
- Mild COPD. Breathing test shows mild airflow
limitation. Signs may include a chronic cough and sputum production. At this
stage, you may not be aware that airflow in your lungs is reduced.
- Moderate COPD. Breathing test shows a worsening
airflow limitation. Usually the signs have increased. Shortness of breath
usually develops when working hard, walking fast, or doing other brisk
activities. At this stage, a person usually seeks medical attention.
- Severe COPD. Breathing test shows severe airflow
limitation. A person is short of breath after just a little activity. In very
severe COPD, complications like respiratory failure or signs of heart failure
may develop. At this stage, the quality of life is greatly impaired and the
worsening symptoms may be life threatening.
Your doctor may also recommend tests to rule out
other causes of your signs and symptoms. These tests include:
- Bronchodilator (brong-ko-di-LA-tor) reversibility
testing. This test uses the spirometer and medicines called bronchodilators.
Bronchodilators work by relaxing tightened muscles around the airways and
opening up airways quickly to ease breathing. Your doctor will use the results
of this test to see if your lung problems are being caused by another lung
condition such as asthma. However, since airways in COPD may also be
constricted, your doctor can use the results of this test to help set your
treatment goals.
- Other pulmonary function testing. For instance,
your doctor could test diffusion capacity.
- Chest x ray. A chest x ray is a picture of your lungs. A chest
x ray may be done to see if another disease, like heart failure, may be causing
your symptoms.
- Arterial blood gas. This is a blood test that
shows the oxygen level in your blood. It is measured in people with severe COPD
to see if oxygen treatment is recommended.
How Is COPD Treated?
Quitting smoking is the single most important thing
you can do to reduce your risk of developing chronic obstructive pulmonary
disease (COPD) and slow the progress of the disease.
Your doctor will recommend treatments that help
relieve your symptoms and help you breathe easier. However, COPD cannot be
cured.
The goals of COPD treatment are to:
- Relieve your symptoms with no or minimal side
effects of treatment
- Slow the progress of the disease
- Improve exercise tolerance (your ability to stay
active)
- Prevent and treat complications and sudden onset
of problems
- Improve your overall health
The treatment for COPD is different for each person.
Your family doctor may recommend that you see a lung specialist called a
pulmonologist (pull-mon-OL-o-gist).
Treatment is based on whether your symptoms are
mild, moderate, or severe.
Medicines and pulmonary rehabilitation (rehab) are
often used to help relieve your symptoms and to help you breathe more easily
and stay active.
COPD Medicines
Bronchodilators
Your doctor may recommend medicines called
bronchodilators that work by relaxing the muscles around your airways. This
type of medicine helps to open your airways quickly and make breathing easier.
Bronchodilators can be either short acting or long acting.
- Short-acting bronchodilators last about 4 to 6
hours and are used only when needed.
- Long-acting bronchodilators last about 12 hours
or more and are used every day.
Most bronchodilator medicines are inhaled, so they
go directly into your lungs where they are needed. There are many kinds of
inhalers, and it is important to know how to use your inhaler correctly.
If you have mild COPD, your doctor may recommend
that you use a short-acting bronchodilator. You then will use the inhaler only
when needed.
If you have moderate or severe COPD, your doctor may
recommend regular treatment with one or more inhaled bronchodilators. You may
be told to use one long-acting bronchodilator. Some people may need to use a
long-acting bronchodilator and a short-acting bronchodilator. This is called
combination therapy.
Inhaled glucocorticosteroids (steroids)
Inhaled steroids are used for some people with
moderate or severe COPD. Inhaled steroids work to reduce airway inflammation.
Your doctor may recommend that you try inhaled steroids for a trial period of 6
weeks to 3 months to see if the medicine is helping with your breathing
problems.
Flu shots
The flu (influenza) can cause serious problems in
people with COPD. Flu shots can reduce the chance of getting the flu. You
should get a flu shot every year.
Pneumococcal vaccine
This vaccine should be administered to those with
COPD to prevent a common cause of pneumonia. Revaccination may be necessary
after 5 years in those older than 65 years of age.
Pulmonary Rehabilitation
Pulmonary rehabilitation (rehab) is a coordinated
program of exercise, disease management training, and counseling that can help
you stay more active and carry out your day-to-day activities. What is included
in your pulmonary rehab program will depend on what you and your doctor think
you need. It may include exercise training, nutrition advice, education about
your disease and how to manage it, and counseling. The different parts of the
rehab program are managed by different types of health care professionals
(doctors, nurses, physical therapists, respiratory therapists, exercise
specialists, dietitians) who work together to develop a program just for you.
Pulmonary rehab programs can include some or all of the following aspects.
Medical evaluation and management
To decide what you need in your pulmonary rehab
program, a medical evaluation will be done. This may include getting
information on your health history and what medicines you take, doing a
physical exam, and learning about your symptoms. A spirometry measurement may
also be done before and after you take a bronchodilator medicine.
Setting goals
You will work with your pulmonary rehab team to set
goals for your program. These goals will look at the types of activities that
you want to do. For example, you may want to take walks every day, do chores
around the house, and visit with friends. These things will be worked on in
your pulmonary rehab program.
Exercise training
Your program may include exercise training. This
training includes showing you exercises to help your arms and legs get
stronger. You may also learn breathing exercises that strengthen the muscles
needed for breathing.
Education
Many pulmonary rehab programs have an educational
component that helps you learn about your disease and symptoms, commonly used
treatments, different techniques used to manage symptoms, and what you should
expect from the program. The education may include meeting with (1) a dietitian
to learn about your diet and healthy eating; (2) an occupational therapist to
learn ways that are easier on your breathing to carry out your everyday
activities; or (3) a respiratory therapist to learn about breathing techniques
and how to do respiratory treatments.
Program results (outcomes)
You will talk with your pulmonary rehab team at
different times during your program to go over the goals that you set and see
if you are meeting them. For example, if your goal is to walk every day for 30
minutes, you will talk to members of your pulmonary team and tell them how
often you are walking and for how long. The team is interested in helping you
reach your goals.
Oxygen Treatment
If you have severe COPD and low levels of oxygen in
your blood, you are not getting enough oxygen on you own. Your doctor may
recommend oxygen therapy to help with your shortness of breath. You may need
extra oxygen all the time or some of the time. For some people with severe
COPD, using extra oxygen for more than 15 hours a day can help them:
- Do tasks or activities with less shortness of
breath
- Protect the heart and other organs from
damage
- Sleep more during the night and improve alertness
during the day
- Live longer
Surgery
For some people with severe COPD, surgery may be
recommended. Surgery is usually done for people who have:
- Severe symptoms
- Not had improvement from taking medicines
- A very hard time breathing most of the time
The two types of surgeries considered in the
treatment of severe COPD are:
- Bullectomy. In this procedure, doctors remove one
or more very large bullae from the lungs of people who have emphysema. Bullae
are air spaces that are formed when the walls of the air sacs break. The air
spaces can become so large that they interfere with breathing.
- Lung volume reduction surgery (LVRS). In this
procedure, surgeons remove sections of damaged tissue from the lungs of
patients with emphysema. A major NHLBI study of LVRS recently showed that
patients whose emphysema was mostly in the upper lobes of the lung and who had
this surgery, along with medical treatment and pulmonary rehabilitation, were
more likely to function better after 2 years than patients who received medical
therapy only. They also did not have a greater chance of dying than the other
patients.
- A small group of these patients
who also had low exercise capacity after pulmonary rehabilitation but before
surgery were also more likely to function better after LVRS than similar
patients who received medical treatment only.
A lung transplant may be done for some people with
very severe COPD. A transplant involves removing the lung of a person with COPD
and replacing it with a healthy lung from a donor.
How Can COPD Be Prevented From Progressing?
If you smoke, the most important thing you can do to
stop more damage to your lungs is to quit smoking. For information on how to
quit smoking, visit the Web site of the
U.S. Office of the Surgeon General. Many hospitals have
smoking cessation programs or can refer you to one.
It is also important to stay away from people who
are smoking and places where you know there will be smokers.
Staying away from other lung irritants such as
pollution, dust, and certain cooking or heating fumes is also important. For
example, you should stay in your house when the outside air quality is poor.
Managing Complications and Preventing Sudden Onset
of Problems
People with chronic obstructive pulmonary disease
(COPD) often have symptoms that suddenly get worse. When this happens, you have
a much harder time catching your breath. You may also have chest tightness,
more coughing, change in your sputum, and a fever. It is important to call your
doctor if you have any of these signs or symptoms.
Your doctor will look at things that might be
causing these signs and symptoms to suddenly worsen. Sometimes the signs and
symptoms are caused by a lung infection. Your doctor may want you to take an
antibiotic medicine that helps fight off the infection.
Your doctor may also recommend additional medicines
to help with your breathing. These medicines include bronchodilators and
glucocorticosteroids.
Your doctor may recommend that you spend time in the
hospital if:
- You have a lot of difficulty catching your
breath.
- You have a hard time talking.
- Your lips or fingernails turn blue or gray.
- You are not mentally alert.
- Your heartbeat is very fast.
- Home treatment of worsening symptoms doesn't
help.
Living With COPD
Although there is no cure for chronic obstructive
pulmonary disease (COPD), your symptoms can be managed, and damage to your
lungs can be slowed. If you smoke, quitting is the most important thing you can
do to help your lungs.
Information is available on ways to help you quit smoking. You
also need to try to stay away from people who are smoking or places where there
is smoking.
It is important to keep the air in your home clean.
Here are some things that may help you in your home:
- Keep smoke, fumes, and strong smells out of your
home.
- If your home is painted or sprayed for insects,
have it done when you can stay away from your home.
- Cook near an open door or window.
- If you heat with wood or kerosene, keep a door or
window open.
- Keep your windows closed and stay at home when
there is a lot of pollution or dust outside.
If you are taking medicines, take them as ordered
and make sure you refill them so you do not run out.
See your doctor at least two times a year, even if
you are feeling fine. Make sure you bring a list of medicines you are taking to
your doctor visit.
Ask your doctor or nurse about getting a flu shot
and pneumonia vaccination.
Keep your body strong by learning breathing
exercises and walking and exercising regularly.
Eat healthy foods. Ask your family to help you buy
and fix healthy foods. Eat lots of fruits and vegetables. Eat protein food like
meat, fish, eggs, milk, and soy.
If your doctor has told you that you have severe
COPD, there are some things that you can do to get the most out of each breath.
Make your life as easy as possible at home by:
- Asking your friends and family for help.
- Doing things slowly.
- Doing things sitting down.
- Putting things you need in one place that is easy
to reach.
- Finding very simple ways to cook, clean, and do
other chores. Some people use a small table or cart with wheels to move things
around. Using a pole or tongs with long handles can help you reach things.
- Keeping your clothes loose.
- Wearing clothes and shoes that are easy to put on
and take off.
- Asking for help moving your things around in your
house so that you will not need to climb stairs as often.
- Picking a place to sit that you can enjoy and
visit with others.
If you are finding that it is becoming more
difficult to catch your breath, your coughing has gotten worse, you are
coughing up more mucus, or you have signs of infection (such as a fever and
feeling poorly), you need to call your doctor right away. Your doctor may do a
spirometry test, blood work, and a
chest x ray. Your doctor may also:
- Order antibiotics, which are medicines that help
fight off infection
- Change the type and dosage of the bronchodilator
and glucocorticosteroid medicines you have been taking
- Order oxygen or increase the amount of oxygen you
are currently using
It is helpful to have certain information on hand in
case you need to go to the hospital or doctor right away. You should plan now
to make sure you have:
- The phone numbers for the doctor, hospital, and
people who can take you to the hospital or doctor
- Directions to the hospital and doctor's
office
- A list of the medicines you are taking
When To Get Emergency Help
You should get emergency help if:
- You find that is hard to talk or walk.
- Your heart is beating very fast or
irregularly.
- Your lips or fingernails are gray or blue.
- Your breathing is fast and hard, even when you
are using your medicines.
Key Points
- Smoking is the most common cause of chronic
obstructive pulmonary disease (COPD).
- COPD is a disease that slowly worsens over time,
especially if you continue to smoke.
- Breathing in other kinds of lung irritants, like
pollution, dust, or chemicals, over a long period of time may also cause or
contribute to COPD. Secondhand smoke and genetic disorders can also play a role
in COPD.
- There is no cure for COPD (which includes
emphysema and chronic bronchitis), and it is a major cause of illness and
death.
- In COPD, much of the elastic quality of the
airways and air sacs in the lung is gone. The airways collapse and obstruct the
normal airflow. Airways may also become inflamed and thickened.
- The signs and symptoms of COPD are different for
each person. Common signs are cough, sputum production, shortness of breath,
wheezing, and chest tightness.
- COPD usually occurs in people who are at least 40
years old. COPD is not contagious.
- If you have COPD, you are more likely to have
lung infections, which can be fatal.
- Your doctor can use a medical history, physical
exam, and breathing tests, such as spirometry, to diagnose—or rule
out—COPD even before you have significant symptoms.
- If the lungs are severely damaged, the heart may
be affected. A person with COPD dies when the lungs and heart are unable to
function and get oxygen to the body's organs and tissues, or when a
complication such as a severe infection occurs.
- Treatment for COPD may help prevent
complications, prolong life, and improve a person's quality of life. Quitting
smoking, staying away from people who are smoking, and avoiding exposure to
other lung irritants are the most important ways to reduce your risk of
developing COPD or to slow the progress of the disease.
- Treatment may include medicines such as
bronchodilators, steroids, flu shots, and pneumococcal vaccine to avoid or
reduce further complications.
- As the symptoms of COPD get worse over time, a
person may have more difficulty with walking and exercising. You should talk to
your doctor about exercising and whether you would benefit from a pulmonary
rehab program—a coordinated program of exercise, physical therapy, disease
management training, advice on diet, and counseling.
- Oxygen treatment and surgery to remove part of a
lung or even to transplant a lung may be recommended for persons with severe
COPD.
- If you have a sudden worsening of signs or
symptoms, it is important to contact your doctor and seek emergency
treatment.
- Be prepared and have information on hand that you
or others would need in a medical emergency, such as information on medicines
you are taking, directions to the hospital or your doctor’s office, and
people to contact if you are unable to speak or call them.
Links to Other Information About COPD
NHLBI Resources
Non-NHLBI Resources
Clinical Trials
|

