What Is an Implantable Cardioverter Defibrillator?
An implantable cardioverter defibrillator (ICD) is a
small device that's placed in your chest or abdomen. This device uses
electrical pulses or shocks to help control life-threatening, irregular
heartbeats, especially those that could lead the heart to suddenly stop beating
(sudden
cardiac arrest). If the heart stops beating, blood stops flowing to the
brain and other vital organs. This usually causes death if it's not treated in
minutes.
The Heart's Electrical System
Your heart has its own internal electrical system
that controls the speed and rhythm of your heartbeat. With each heartbeat, an
electrical signal spreads from the top of the heart to the bottom. As it
travels, the electrical signal causes the heart to contract and pump blood.
Electrical signals normally begin in a group of
cells called the sinus node. As these signals spread from the top to the bottom
of the heart, they coordinate the timing of heart cell activity. First, the two
upper chambers of the heart, called atria (AY-tree-uh), contract. This
contraction squeezes blood into the lower chambers of the heart, which are
called ventricles (VEN-trih-kuls). The ventricles then contract and send blood
to the rest of the body. The combined contraction of the atria and ventricles
is a heartbeat.
For more information about the heart's electrical
system and how a healthy heart works, see the Diseases and Conditions Index
article on
How
the Heart Works.
Overview
A problem with any part of the electrical system
process can cause irregular heartbeats called
arrhythmias
(ah-RITH-me-ahs). During an arrhythmia, the heart can beat too fast, too slow,
or with an irregular rhythm. Faulty electrical signaling in the heart causes
arrhythmias.
ICDs use electrical pulses or shocks to treat
life-threatening arrhythmias that occur in the ventricles (lower chambers of
the heart).
When these ventricular arrhythmias occur, the heart
can't effectively pump blood, and a person will pass out within seconds and die
within minutes if not treated. To prevent death, the condition must be treated
right away with an electric shock to the heart. This treatment is called
defibrillation.
An ICD has wires with electrodes on the ends that
connect to the chambers of your heart. The ICD will continually monitor your
heart rhythm. When the device detects that you're having an irregular rhythm in
your ventricles, the ICD will use low-energy electrical pulses to restore a
normal rhythm. If this doesn't restore your normal heart rhythm, or if your
ventricles start to quiver rather than contract strongly, the ICD will switch
to high-energy electrical pulses for defibrillation.
Doctors also treat irregular heartbeats with another
device called a pacemaker. An ICD is similar to a pacemaker, but there are some
differences. Pacemakers can only give off low-energy electrical pulses. They
are often used to treat less dangerous heart rhythms, such as those that occur
in the upper chambers of your heart. Most new ICDs can act as both pacemakers
and ICDs.
Comparison of an Implantable
Cardioverter Defibrillator
and a Pacemaker
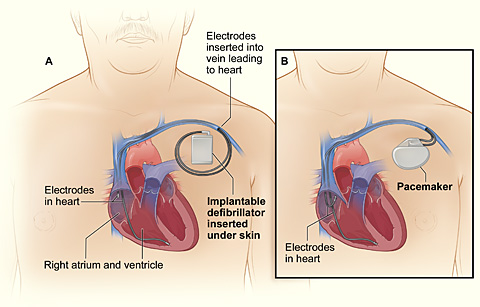
The illustration compares an
implantable cardioverter defibrillator and a pacemaker. Figure A shows the
location and general size of an implantable cardiac defibrillator in the upper
chest. The wires with electrodes on the ends are inserted into the heart
through a vein in the upper chest. Figure B shows the location and general size
of a double-electrode pacemaker in the upper chest. The wires with electrodes
on the ends are inserted into the heart through a vein in the upper chest.
For more information, see the Diseases and
Conditions Index article on
Pacemaker.
Who Needs an Implantable Cardioverter
Defibrillator?
You may need an implantable cardioverter
defibrillator (ICD) if you're at risk for certain life-threatening ventricular
arrhythmias,
such as ventricles that beat too fast or that quiver. For example, you may be
considered at high risk for a ventricular arrhythmia if you:
- Have had a ventricular arrhythmia before
- Have had a
heart
attack that has damaged the electrical system in your ventricles
An ICD is often recommended for people who have
survived
sudden
cardiac arrest.
Your doctor may recommend an ICD if he or she sees
signs of a ventricular arrhythmia (or heart damage that would make one likely)
on the following tests.
Electrocardiogram
This simple and painless test detects and records
the electrical activity of the heart. An
EKG
(electrocardiogram) shows how fast the heart is beating and the heart's rhythm
(steady or irregular). It also records the strength and timing of electrical
signals as they pass through each part of the heart.
Holter Monitor
A
Holter monitor, also called an ambulatory EKG, records the
electrical signals of your heart for a full 24- or 48-hour period. You wear
small patches called electrodes on your chest that are connected by wires to a
small, portable recorder. The recorder can be clipped to a belt, kept in a
pocket, or hung around your neck.
During the 24 or 48 hours, you do your usual daily
activities and keep a notebook, writing down any symptoms you have and the time
they occur. You then return both the recorder and the notebook to your doctor
to read the results. Your doctor can see how your heart was beating at the time
you had symptoms.
The purpose of a Holter monitor is to record heart
signals during typical daily activities and while sleeping, and to find heart
problems that may occur for only a few minutes out of the day. Also, the Holter
monitor can pick up irregular heartbeats that don't cause symptoms, but are
important to treat.
Echocardiogram
This test uses sound waves to create a moving
picture of your heart. An
echocardiogram
provides information about the size and shape of your heart and how well your
heart chambers and valves are working. The test also can identify areas of poor
blood flow to the heart, areas of heart muscle that aren't contracting
normally, and injury to the heart muscle caused by poor blood flow.
Electrophysiology Study
For an
electrophysiology study, your doctor threads a catheter (a
small, flexible tube) from a blood vessel in your arm or leg up to your heart.
Through the catheter, your doctor gives you certain medicines and electrically
stimulates your heart to see how your heart's electrical system responds. The
electrical stimulation helps to find where the heart 's electrical system is
damaged.
Stress Test
Some heart problems are easier to diagnose when
your heart is working harder and beating faster than when it's at rest. During
stress
testing, you exercise (or are given medicine if you are unable to exercise)
to make your heart work harder and beat faster while heart tests, such as an
EKG or echocardiogram, are performed.
How Does an Implantable Cardioverter Defibrillator
Work?
An implantable cardioverter defibrillator (ICD) has
wires with electrodes on the ends that connect to one or more of your heart's
chambers. These wires monitor your heart rhythm. They also deliver high- or
low-energy electrical pulses to the heart when it beats abnormally.
Single-chamber ICDs have wires that connect to one
or both of your ventricles. These ICDs correct faulty electrical signaling
within the ventricles. Dual-chamber ICDs have wires that connect to both an
upper heart chamber (atrium) and a ventricle. These ICDs correct faulty
electrical signaling between the two chambers.
The wires on an ICD connect to a small metal box
implanted in your chest or abdomen that contains a battery, pulse generator,
and computer. The computer triggers the ICD's pulse generator to send
electrical pulses when it detects irregular rhythms. Wires carry these pulses
to the heart.
The ICD also can record the heart's electrical
activity and heart rhythms. The recordings can help your doctor fine-tune the
programming of your ICD so it works better to correct irregular heartbeats.
Whether you receive a single-chamber or
dual-chamber ICD is based on your heart's pumping abilities, structural
defects, and the type of irregular heartbeats you've had. Whichever type of ICD
you receive, it will be programmed to respond to the type of irregular heart
rhythm you're most likely to have.
What To Expect During Implantable Cardioverter
Defibrillator Surgery
Placing an implantable cardioverter defibrillator
(ICD) requires minor surgery, which is usually done in a hospital. You will be
given medicine right before the surgery that will help you relax and may make
you fall asleep. Your doctor will give you a local anesthetic so you won't feel
anything in the area where he or she puts the ICD.
First, your doctor will thread the ICD wires
through a vein to the correct location in your heart. An x-ray "movie" of the
wires as they pass through your vein and into your heart will help your doctor
place the wires. Once the wires are in place, your doctor will make a small cut
into the skin of your chest or abdomen. He or she will then slip the
generator/battery box part of the ICD through the cut and place it just under
your skin.
Once in place, your doctor will test your ICD. You
will be given medicine to help you sleep during this testing so you don't feel
any electrical pulses. Then your doctor will sew up the cut. The entire surgery
takes a few hours.
What To Expect After Implantable Cardioverter
Defibrillator Surgery
Expect to stay in the hospital 1 to 2 days so your
heartbeat can be monitored and your doctor can make sure your implantable
cardioverter defibrillator (ICD) is working properly. You may need to arrange
for a ride home from the hospital. Check with your doctor about whether you can
drive after the procedure.
For a few days to weeks after surgery, you may have
pain, swelling, or tenderness in the area where your ICD was placed. The pain
is usually mild, and over-the-counter medicines can help relieve it. Consult
with your doctor before taking any pain medicines. Your doctor also may ask you
to avoid any vigorous activities and heavy lifting for about a month. Most
people return to normal activities within a few days of having ICD surgery.
What Are the Risks of Having an Implantable
Cardioverter Defibrillator?
The most common problem with implantable
cardioverter defibrillators (ICDs) is that they give pulses when they aren't
needed. Pulses delivered too often or at the wrong time can damage the heart or
trigger an irregular heartbeat. They also can be painful and emotionally
upsetting. If this occurs, your doctor can reprogram the ICD or prescribe
medicines so the pulses occur less often.
Although rare, some risks are linked to the ICD
surgery, including:
- Swelling, bruising, or infection in the area
where the ICD was placed
- Bleeding from the site where the ICD was placed
- Blood vessel, heart, or nerve damage
- A collapsed lung
- A bad reaction to the medicine used to make you
sleep during the surgery
People with an ICD may be at increased risk of
developing
heart
failure. Heart failure is when your heart can't pump enough blood
throughout the body. It's not known for sure whether an ICD increases the risk
of heart failure or whether heart failure is just more common in people who
need an ICD.
There also is the rare risk that your ICD won't
work correctly. This will prevent your ICD from correcting irregular heart
rhythms. If your ICD malfunctions, your doctor may be able to reprogram it. If
that doesn't work, the ICD may need to be replaced.
How Will an Implantable Cardioverter Defibrillator
Affect my Lifestyle?
The low-energy electrical pulses your implantable
cardioverter defibrillator (ICD) gives off aren’t painful. You may not
notice them,or you may feel a fluttering in your chest.
The high-energy pulses your ICD gives last only a
second and feel like a thumping or painful kick in the chest, depending on
their strength. Your doctor may give you medicine to lower the number of
irregular heartbeats you have. This will reduce the number of high-energy
pulses sent to your heart. Such medicines include amiodarone or sotalol and
beta blockers.
Your doctor may want you to call his or her office
or come in within 24 hours of getting a strong shock from your ICD. See your
doctor or go to an emergency room right away if you get many strong pulses
within a short time.
Devices That Can Disrupt Implantable Cardioverter
Defibrillator Functions
Once you have an ICD, you have to avoid close or
prolonged contact with electrical devices or devices that have strong magnetic
fields. Devices that can interfere with an ICD include:
- Cell phones
- iPods
- Appliances, such as microwave ovens
- High-tension wires
- Metal detectors
- Industrial welders
- Electrical generators
These devices can disrupt the electrical signaling
of your ICD and stop it from working properly. You may not be able to tell
whether your ICD has been affected. How likely a device is to disrupt your ICD
depends on how long you’re exposed to it and how close it is to your ICD.
To be on the safe side, some experts recommend not
putting your cell phone or iPod in a shirt pocket over your ICD (if they are
turned on). You may want to hold your cell phone up to the ear that’s
opposite the site where your ICD was implanted. If you strap your iPod to your
arm while listening to it, put it on the arm farthest from your ICD.
You can still use household appliances, but avoid
close and prolonged exposure, as it may interfere with your ICD.
You can walk through security system metal
detectors at your normal pace. Someone can check you with a metal detector wand
as long as it isn’t held for too long over your ICD site. You should avoid
sitting or standing close to a security system metal detector.
Stay at least 2 feet away from industrial welders
or electrical generators.
Some medical procedures also can disrupt your ICD.
These procedures include:
- Magnetic resonance imaging (also called MRI)
- Shock-wave lithotripsy to get rid of kidney
stones
- Electrocauterization to stop bleeding during
surgery
Let all of your doctors, dentists, and medical
technicians know that you have an ICD. You also should notify airport
screeners. Your doctor can give you a card that states what kind of ICD you
have. Carry this card in your wallet.
Maintaining Daily Activities
Physical Activity
In most cases, having an ICD won’t limit you
from taking part in sports and exercise, including strenuous activities. You
may need to avoid full-contact sports, such as football. Such contact could
damage your ICD or shake loose the wires in your heart. Ask your doctor how
much and what kinds of physical activity are safe for you.
Driving
An ICD will not prevent you from driving. However,
your doctor may ask you not to drive until you have gone 6 months without
fainting. Some people may still faint even with an ICD.
Followup
Your doctor will want to check your ICD regularly.
Over time, your ICD may stop working properly because:
- Its wires get dislodged or broken
- Its battery fails
- Your heart disease progresses
- Other devices have disrupted its electrical
signaling
To check your ICD, your doctor may ask you to come
in for an office visit several times a year. Some ICD functions can be checked
remotely through a telephone call or a computer connection to the Internet.
Your doctor also may ask you to have an
EKG (electrocardiogram) to check for changes in the electrical activity of
your heart.
Battery Replacement
ICD batteries last between 5 and 7 years. Your
doctor will replace the generator along with the battery before the battery
begins to run down.
Replacing the generator/battery is less involved
surgery than the original surgery to implant the ICD. The wires of your ICD
also may need to be replaced eventually. Your doctor can tell you whether you
need to replace your ICD or its wires.
What Are the Benefits of Having an Implantable
Cardioverter Defibrillator?
An ICD is very effective in detecting and stopping
certain deadly heart rhythms. An ICD can be more effective than drug therapy in
preventing
sudden
cardiac arrest, depending on the cause of the arrest. Although an ICD can't
cure heart disease, it can lower the risk of dying by up to 50 percent in some
patients who have heart disease.
Key Points
- An implantable cardioverter defibrillator (ICD)
is a small device that's placed in your chest or abdomen to help control
life-threatening, irregular heart rhythms (called
arrhythmias).
- An ICD has wires with electrodes that connect to
one or more of your heart's chambers. The ICD will continually monitor your
heart rhythm. The device also will deliver high- or low-energy electrical
pulses or shocks to the heart when it beats irregularly.
- An ICD isn't the same as a
pacemaker.
A pacemaker can only give off low-energy electrical pulses to correct certain
irregular heartbeats. An ICD can give off the high-energy electrical pulses
needed to correct dangerous arrhythmias in the lower chambers of the heart
(ventricles).
- Your doctor may recommend an ICD if he or she
sees signs of an irregular ventricular arrhythmia (or heart damage that would
make one likely). He or she also may recommend an ICD if you survive
sudden
cardiac arrest.
- Surgery to place an ICD usually takes a few
hours. After this minor surgery, you may have mild pain; over-the-counter
medicines can usually relieve it. Consult your doctor before taking any pain
medicine.
- The most common problem with ICDs is that they
give pulses too often or when they aren't needed. Doctors can reprogram ICDs or
prescribe medicines so the pulses occur less often. There are other rare risks
linked to the ICD surgery, such as infection and bleeding.
- The low-energy electrical pulses your ICD gives
off aren't painful. You may not notice them, or you may feel a fluttering in
your chest.
- The high-energy pulses your ICD gives only last
a second and feel like a thumping or painful kick in the chest, depending on
their strength. Your doctor may give you medicine to lower the number of
arrhythmias
you have. This may reduce the number of high-energy pulses sent to your heart.
- Once you have an ICD, you have to avoid close or
prolonged contact with electrical devices or devices that have strong magnetic
fields. You also need to avoid medical procedures that can disrupt your ICD.
- Let all of your doctors, dentists, and medical
technicians know that you have an ICD.
- Your doctor may ask you to avoid any vigorous
exercise or heavy lifting for a short period after your surgery. After you have
fully recovered from surgery, discuss with your doctor how much and what kinds
of physical activity are safe for you.
- Have your ICD checked regularly. Some ICD
functions can be checked remotely through a telephone call or computer
connection to the Internet. Your doctor may ask you to come to his or her
office to check your ICD.
- ICD batteries have to be replaced every 5 to 7
years. The wires of your ICD also may have to be replaced eventually. You
doctor can tell you whether you need to replace your ICD or its wires.
Links to Other Information About Pacemaker
NHLBI Resources
Non-NHLBI Resources
Clinical Trials
|

