What Is Patent Ductus Arteriosus?
Patent ductus arteriosus (PDA) is a heart problem
that occurs soon after birth in some babies. In PDA, there is an abnormal
circulation of blood between two of the major arteries near the heart. Before
birth, the two major arteries—the aorta and the pulmonary artery—are
normally connected by a blood vessel called the ductus arteriosus, which is an
essential part of the fetal circulation. After birth, the vessel is supposed to
close within a few days as part of the normal changes occurring in the baby's
circulation. In some babies, however, the ductus arteriosus remains open
(patent). This opening allows blood to flow directly from the aorta into the
pulmonary artery, which can put a strain on the heart and increase the blood
pressure in the lung arteries.
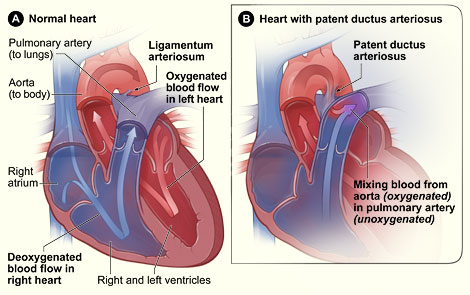
Figure A shows the normal anatomy
and blood flow of the interior of the heart. Figure B shows a heart with a
patent ductus arteriosus. The defect connects the aorta with the pulmonary
artery, allowing oxygen-rich blood from the aorta to mix with oxygen-poor blood
in the pulmonary artery.
A PDA is a type of
congenital
heart defect. A congenital heart defect is any type of heart problem that
is present at birth.
If your baby has a PDA, but has an otherwise normal
heart, the PDA may shrink and go away completely, or it may need to be treated
to close it. But, if your baby is born with certain types of heart defects that
decrease blood flow from the heart to the lungs or the body, medicine may be
given to keep the ductus arteriosus open to maintain blood flow and oxygen
levels until corrective surgery for the heart defect(s) can be performed.
About 3,000 infants are diagnosed with PDA each year
in the United States. It is more common in premature infants (babies born too
early) but does occur in full-term infants. Premature babies with PDA are more
vulnerable to its effects. PDA is twice as common in girls as in boys.
The next section, How
the Heart Works, provides a more detailed description of a heart with a PDA
compared to a normal heart. See that section for a more detailed description of
the anatomy and circulation of a normal heart.
How the Heart Works
Your child’s heart is a muscle about the size
of his or her fist. It works like a pump and beats 100,000 times a day.
The heart has two sides, separated by an inner wall
called the septum. The right side of the heart pumps blood to the lungs to pick
up oxygen. Then, oxygen-rich blood returns from the lungs to the left side of
the heart, and the left side pumps it to the body.
The heart has four chambers and four valves and is
connected to various blood vessels. Veins are the blood vessels that carry
blood from the body to the heart. Arteries are the blood vessels that carry
blood away from the heart to the body.
A Healthy Heart Cross-Section
The illustration shows a
cross-section of a healthy heart and its inside structures. The blue arrow
shows the direction in which oxygen-poor blood flows from the body to the
lungs. The red arrow shows the direction in which oxygen-rich blood flows from
the lungs to the rest of the body.
Heart Chambers
The heart has four chambers or "rooms."
- The atria (AY-tree-uh) are the two upper chambers
that collect blood as it comes into the heart.
- The ventricles (VEN-trih-kuls) are the two lower
chambers that pump blood out of the heart to the lungs or other parts of the
body.
Heart Valves
Four valves control the flow of blood from the atria
to the ventricles and from the ventricles into the two large arteries connected
to the heart.
- The tricuspid (tri-CUSS-pid) valve is in the
right side of the heart, between the right atrium and the right ventricle.
- The pulmonary (PULL-mun-ary) valve is in the
right side of the heart, between the right ventricle and the entrance to the
pulmonary artery, which carries blood to the lungs.
- The mitral (MI-trul) valve is in the left side
of the heart, between the left atrium and the left ventricle.
- The aortic (ay-OR-tik) valve is in the left side
of the heart, between the left ventricle and the entrance to the aorta, the
artery that carries blood to the body.
Valves are like doors that open and close. They open
to allow blood to flow through to the next chamber or to one of the arteries,
and then they shut to keep blood from flowing backward.
When the heart's valves open and close, they make a
"lub-DUB" sound that a doctor can hear using a stethoscope.
- The first sound—the “lub”—is
made by the mitral and tricuspid valves closing at the beginning of systole
(SIS-toe-lee). Systole is when the ventricles contract, or squeeze, and pump
blood out of the heart.
- The second sound—the “DUB”—is
made by the aortic and pulmonary valves closing at beginning of diastole
(di-AS-toe-lee). Diastole is when the ventricles relax and fill with blood
pumped into them by the atria.
Arteries
The arteries are major blood vessels connected to
your heart.
- The pulmonary artery carries blood pumped from
the right side of the heart to the lungs to pick up a fresh supply of
oxygen.
- The aorta is the main artery that carries
oxygen-rich blood pumped from the left side of the heart out to the body.
- The coronary arteries are the other important
arteries attached to the heart. They carry oxygen-rich blood from the aorta to
the heart muscle, which must have its own blood supply to function.
Veins
The veins are also major blood vessels connected to
your heart.
- The pulmonary veins carry oxygen-rich blood from
the lungs to the left side of the heart so it can be pumped out to the
body.
- The vena cava is a large vein that carries
oxygen-poor blood from the body back to the heart.
For more information on how a healthy heart works,
see the Diseases and Conditions Index article on
How
the Heart Works. This article contains animations that show how your heart
pumps blood and how your heart’s electrical system works.
The Heart With Patent Ductus Arteriosus
The ductus arteriosus is a blood vessel that
connects a baby's aorta and pulmonary artery while the baby is in the womb.
This connection allows blood to be pumped from the right side of the heart
straight to the aorta without stopping at the lungs for oxygen. In the womb,
only a small amount of a baby's blood needs to go to the lungs because the baby
gets oxygen from the mother's bloodstream. The baby's pulmonary artery, which
carries blood to the lungs, is not needed at this time.
After birth, the baby is no longer connected to the
mother's bloodstream. The baby's blood must now go to his or her own lungs to
get oxygen. Normally, as the baby begins to breathe on his or her own, the
pulmonary artery opens to allow blood into the lungs, and the ductus arteriosus
closes. Once the ductus arteriosus closes, blood leaving the right side of the
heart no longer goes straight to the aorta. First, it goes through the
pulmonary arteries and stops at the lungs to pick up oxygen. Then, blood
carrying oxygen returns to the left side of the heart and is pumped out to the
rest of the body.
If the ductus arteriosus does not close after birth
as it should, it is called a patent ductus arteriosus (PDA). A PDA allows blood
to flow directly from the aorta into the pulmonary artery and from there to the
lungs. This extra amount of blood flowing into the lungs strains the heart and
increases the blood pressure in the arteries of the lungs.
Effects of patent ductus arteriosus
Normal birth-weight infants. The
larger a PDA is, the greater the amount of extra blood that passes through the
lungs. A small PDA might not cause any problems, whereas a larger PDA is likely
to cause problems.
PDA can increase the risk of
bacterial endocarditis. Bacterial endocarditis is an infection
of the lining of the heart, valves, or arteries. In the case of PDA, the
increased flow of blood can irritate the lining of the pulmonary artery where
the PDA connects. This irritation makes it easier for bacteria in the
bloodstream to collect and grow there.
A large PDA that is allowed to remain open for an
extended period of time can cause the heart to enlarge and to have to work
harder. Also, fluid can build up in the lungs.
Premature infants. For premature
infants (babies born too early), PDA can be more serious than in normal-weight
babies. Preemies with PDA are more likely to have damage to their lungs from
the extra blood flowing through the PDA. Preemies with PDA may need to be on a
ventilator to help them with their breathing.
The increased flow of blood through the lungs also
can reduce blood flow to the rest of the body. This can damage other organs,
especially the intestines and kidneys.
What Causes Patent Ductus Arteriosus?
The cause of patent ductus arteriosus (PDA) is not
known.
Genetics may play a role. A defect in one or more
genes could prevent the ductus arteriosus from closing normally after
birth.
PDA is more common in:
- Premature infants (babies born too early)
- Infants with genetic abnormalities such as Down
syndrome
- Infants whose mother had German measles (rubella)
during pregnancy
What Are the Signs and Symptoms of Patent Ductus
Arteriosus?
A
heart
murmur may be the only sign that a baby has patent ductus arteriosus (PDA).
A heart murmur is an extra or unusual sound heard during the heartbeat.
Some infants may develop signs or symptoms of volume
overload on the heart and excess blood flow in the lungs. Signs and symptoms
may include:
- Fast breathing, working hard to breathe, or
shortness of breath, or in the case of a premature infant, need for increased
oxygen or ventilatory support
- Poor feeding and poor weight gain
- Tiring easily
- Sweating with exertion (such as while
feeding)
How Is Patent Ductus Arteriosus Diagnosed?
In full-term infants, a patent ductus arteriosus
(PDA) usually is first suspected when the baby's doctor hears a heart murmur
during a regular checkup. If a PDA is large, the infant may also develop
symptoms of volume overload and increased blood flow to the lungs. When a PDA
is small, it may not be diagnosed until later in childhood. Once a PDA is
suspected, a consultation with a pediatric cardiologist will be arranged. A
pediatric cardiologist is a doctor who specializes in diagnosing and treating
heart problems in children.
In premature babies (babies born too early) with
PDA, the physical signs that are seen in full-term babies, such as heart
murmur, may not be present. Doctors may suspect a PDA in premature babies who
develop breathing difficulties soon after birth. Doctors use tests such as
echocardiography to look for PDA in premature babies with breathing
problems.
Tests
Two painless tests are used to diagnose a PDA.
- Echocardiogram. This test, which is harmless and painless,
uses sound waves to create a moving picture of your baby's heart. During an
echocardiogram, reflected sound waves outline the heart's structure completely.
The test allows the doctor to clearly see any problem with the way the heart is
formed or the way it's working. An echocardiogram is the most important test
available to your baby's cardiologist to both diagnose a heart problem and
follow the problem over time. In babies with PDA, the echocardiogram shows how
big the ductus is and how well the heart is responding to it. When medical
treatments are used to try to close a ductus in premature babies,
echocardiograms are used to see how well the treatment is working.
- EKG
(electrocardiogram). This test records the electrical activity in the heart. In
the case of a PDA, it can show:
- Enlargement of the heart chambers
- Other subtle changes that can suggest the
presence of a PDA
How Is Patent Ductus Arteriosus Treated?
The goal of treatment is to close the patent ductus
arteriosus (PDA) to prevent complications and reverse the effects of increased
blood volume.
Small PDAs often close without treatment. For
full-term infants, treatment is needed if the child's PDA:
- Is large
- Is causing the child to have health problems
- Does not close on its own by the time the child
is 1–2 years old
For premature infants (babies born too early),
treatment is needed if the PDA is causing increased respiratory distress and
heart problems.
Specific Types of Treatment
Treatments for PDA include:
- Medicines
- Catheter-based procedures
- Surgery
Your child's doctor will discuss the treatment
options and your family's preferences regarding treatment decisions.
Medicines
Medicines can be given to help close a PDA.
- Indomethacin (in-doh-METH-ah-sin) is a drug that helps close a
PDA in premature infants. It does not usually work in full-term infants. It
works by stimulating the PDA to constrict or tighten, closing the
connection.
- Ibuprofen (EYE-boo-pro-fen) is a medicine in the same family
as indomethacin. It is also used frequently to close a PDA in premature
infants.
If a PDA is small and the decision is made not to
treat it right away, antibiotics may be prescribed to prevent
endocarditis.
Catheter-based procedures
Catheters are thin, flexible tubes used in a
procedure called
cardiac
catheterization (KATH-e-ter-i-ZA-shun). Catheter-based procedures are often
used to close PDAs in infants or children who are large enough to have the
procedure. Your child's doctor may refer to the procedure as "transcatheter
device closure." The procedure is sometimes done on small PDAs to prevent the
risk of bacterial endocarditis.
During the procedure, your child will be sedated or
given general anesthesia so he or she will sleep and not feel any discomfort.
The doctor will place a catheter in a large blood vessel in the upper thigh
(groin) and guide it to your child's heart.
A small metal coil or other blocking device is
passed up through the catheter and placed in the ductus arteriosus to block
blood flow through the vessel.
Catheter-based procedures:
- Do not require the child's chest to be
opened
- Let the child recover quickly
Closing a PDA using a catheter is often done on an
outpatient basis. You will most likely be able to take your child home the same
day the procedure is done.
Complications of catheter-based procedures are rare
and short term. They can include bleeding, infection, and movement of the
blocking device from where it was placed.
Surgery
Surgery for PDA may be performed when:
- A premature or full-term infant develops health
problems from the PDA and is too small to have a catheter-based procedure
- A PDA is not successfully closed by a
catheter-based procedure
- Surgery is planned for treatment of related
congenital
heart defects
Surgery often is not performed until after 6 months
of age in infants who do not have health problems from the PDA. Doctors
sometime perform surgery on small PDAs to prevent the risk of bacterial
endocarditis.
The operation is done under general anesthesia so
that your child will sleep and not feel any pain. The surgeon will:
- Make a small cut between your child's ribs to
reach the PDA
- Close the PDA with stitches or clips
Complications of the surgery are rare and usually
short term. They can include hoarseness, a paralyzed diaphragm, infection,
bleeding, or fluid buildup around the lungs.
After surgery. After surgery, your
child will spend a few days in the hospital. Most children go home 2 days after
surgery. While in the hospital, your child will be given medicines to reduce
pain or anxiety. The doctors and nurses at the hospital will teach you how to
care for your child at home. They will talk to you about:
- Limits on activity for your child while he or she
recovers
- Followup appointments with your child's
doctors
- How to give your child medicines at home, if
needed
When your child goes home after surgery, you can
expect that he or she will feel fairly comfortable, although there may be some
pain temporarily.
Your child should begin to eat better and gain
weight quickly. Within a few weeks, your child should be fully recovered and
able to participate in normal activities.
Long-term complications from surgical treatment are
rare. They can include narrowing of the aorta, incomplete closure of the ductus
arteriosus, and reopening of the ductus arteriosus.
Living With Patent Ductus Arteriosus
Most children are healthy and live normal lives
after treatment for a patent ductus arteriosus (PDA).
If your child was not born prematurely (too early),
he or she is expected to have normal activity levels, appetite, and growth
after PDA treatment, as long as there are no other
congenital
heart defects.
If your child was born prematurely, the outlook
after PDA treatment depends primarily on other factors, such as:
- How early he or she was born
- Whether he or she has other illnesses or
conditions, such as other congenital heart defects
Medical Care Needs
Children who have PDAs are at increased risk for
bacterial endocarditis. To prevent this infection, your doctor
may give your child antibiotics before medical or dental procedures (such as
surgery or dental cleanings) that could allow bacteria into the bloodstream.
Talk to you child's doctor about whether your child needs antibiotics before
such procedures.
It's important to take good care of your child's
teeth. He or she should have regular dental care to prevent decay and help
reduce the chance of infection.
Once the PDA is closed, your child will not need
antibiotics before dental work or surgical procedures. If the PDA is closed
surgically or by catheter and remains completely closed, antibiotics will not
be needed after 6 months.
Key Points
- Patent ductus arteriosus (PDA) is a persistent
connection between the aorta and the pulmonary artery after birth. This
connection is called the ductus arteriosus, and it is normally present before
birth. In most babies, the vessel closes within a few hours to days after
birth. In some babies, the ductus arteriosus remains open (patent) after
birth.
- PDA is more common in premature infants (babies
born too early), but it can happen in full-term infants. It is twice as common
in girls as in boys.
- The cause of PDA is not known. Genetics may play
a role. PDA can occur in children with otherwise normal hearts or in children
born with other heart defects.
- PDA allows too much blood to pump through the
lungs, overloading the heart and the lungs. The heart must work harder than
usual to pump the extra blood. This can cause the heart to enlarge and fluid to
increase in the lungs.
- PDA can lead to poor growth, damage to the
arteries in the lungs due to the extra blood flow, and
bacterial endocarditis.
- A
heart
murmur may be the only sign that a baby or child has a PDA.
- Some infants may develop signs and symptoms of a
large PDA such as fast breathing, poor feeding and poor weight gain, tiring
easily, and sweating.
- Children with a large PDA are usually diagnosed
within the first few months of life. Children with a small PDA may not be
diagnosed until they are older. Premature infants with PDA may be diagnosed
soon after birth.
- The
echocardiogram is the test most commonly used to confirm the
presence of a PDA.
- Small PDAs sometimes close without treatment. But
if a PDA is large or does not close on its own by the time the child is
1–2 years old, it should be repaired. For premature infants, treatment is
needed if the PDA is causing increased respiratory distress and heart
problems.
- Treatments for PDA include medicine, procedures
using catheters, and surgery.
- After closure of a PDA, most children grow
normally and live healthy lives.
Links to More Information About Patent Ductus
Arteriosus
NHLBI Resources
Non-NHLBI Resources
Clinical Trials
|

