| 
Cholesterol Drugs Lower Stroke Risk in Older People
 WEDNESDAY, Sept. 3 (HealthDay News) -- Taking a cholesterol-lowering drug after a stroke or mini-stroke reduces an older person's risk of another stroke much as it does in younger patients, according to a U.S. study.
"Even though the majority of strokes and heart attacks occur in people who are 65 and older, studies have found that cholesterol-lowering drugs are not prescribed as often for older people as they are for younger people. These results show that using these drugs is just as beneficial for people who are 65 as they are for younger people," study author Dr. Seemant Chaturvedi, of Wayne State University in Detroit, said in an American Academy of Neurology news release.
The researchers looked at 4,731 people who had had a recent stroke or mini-stroke (transient ischemic attack), including 2,249 people age 65 and older and 2,482 people under age 65. In each group, about half the patients received the cholesterol-lowering drug atorvastatin (Lipitor), and about half received a placebo. The participants were then followed for an average of 4.5 years.
Levels of "bad" low-density lipoprotein (LDL) cholesterol were reduced by an average of 61 points in the over-65 group and by an average of 59 point in the under-65 group. Stroke risk was reduced by 26 percent in the younger group and by 10 percent in the older group, the study found.
"We tested to see whether age had any effect on how well the treatment worked, and we did not find any differences between young people and older people," Chaturvedi said. "It's estimated that 20 percent of the U.S. population will be 65 or older by 2010, so it's important that we identify ways to reduce the burden of strokes and other cerebrovascular diseases in this group. This is a step in that direction."
The study, which was supported by atorvastatin maker Pfizer Inc., was published in the Sept. 3 online issue of the journal Neurology.
More information
The U.S. National Institute of Neurological Disorders and Stroke has more about stroke.
|  |

Most Patients With Irregular Heartbeat Take Inadequate Blood Thinner Dose
 THURSDAY, Aug. 28 (HealthDay News) -- Only 40 percent of patients with atrial fibrillation, a known risk factor for stroke, who did suffer a stroke were taking the anti-clotting drug warfarin, a new study found.
Among those taking warfarin, 75 percent weren't getting the dose needed to prevent a stroke. And an additional 25 percent were taking medications that were less effective at preventing clots or no medication at all, according to the report by Canadian researchers.
"These are missed opportunities for stroke prevention," lead researcher Dr. David J. Gladstone, a stroke neurologist at the University of Toronto, said in a prepared statement. "Sadly, we frequently see patients admitted to a hospital with a devastating stroke who are known to have atrial fibrillation, yet were either not taking warfarin or were taking a dose that is not therapeutic. We consider these to be potentially preventable strokes."
The findings are published online Aug. 29 in the journal Stroke.
Gladstone's team collected data on 2,135 stroke patients listed in the Registry of the Canadian Stroke Network. Among these patients, 597 were diagnosed with atrial fibrillation, an irregular heartbeat, before their stroke. For these patients, 60 percent of the strokes were disabling, and 20 percent were fatal.
Warfarin, by thinning the blood, helps prevent clots from developing and reduces the risk of stroke by about 67 percent in people with atrial fibrillation (AF). Strokes caused by AF can be more severe than other strokes, and studies have shown that warfarin can reduce the severity of strokes in patients with atrial fibrillation, the researchers said.
It's not clear why the rates of warfarin use were so low, the researchers said. "On one hand, we have an extremely effective and cheap medication for stroke prevention -- warfarin -- yet, on the other hand, it remains under-used in people who would benefit most from it," Gladstone said.
The study authors believe that efforts are needed to educate physicians and patients about the benefits of warfarin therapy for those with atrial fibrillation. "This is a public health priority, because atrial fibrillation is one of the most common causes of stroke," Gladstone said. "Many more strokes could be prevented if anti-coagulation therapy were optimized in the population at large."
Dr. Byron Lee, an assistant professor of cardiology at the University of California, San Francisco, thinks part of the problem may owe to the fact that many patients have problems taking warfarin, because it requires blood tests to monitor its effectiveness. Too low a dose is ineffective, while too high a dose can cause internal bleeding. So, patients need to have their warfarin levels measured at least once a month, he said.
"Patients hate taking warfarin, and doctors hate prescribing it," Lee said. "This is mainly because it's a hassle. However, this study confirms that many strokes can be avoided if patients are adequately anti-coagulated. Therefore, both patients and doctors need to do a better job of overcoming the inconvenience of warfarin."
Dr. John Worthington is a stroke physician at Liverpool and Northern Beaches Hospitals at the University of New South Wales in Sydney, Australia, who wrote an accompanying editorial in the journal. He said it's essential for patients with atrial fibrillation to receive warfarin to prevent a stroke.
"Warfarin is usually the best and safest available treatment to prevent stroke in people with atrial fibrillation. Increasing the uptake of warfarin would reduce the risk of death and disability of stroke," he said.
Worthington said patients with AF should ask their doctor why they aren't being prescribed warfarin.
More information
To learn more about atrial fibrillation visit the American Heart Association  . .
|  |

Strokes Can Strike the Youngest
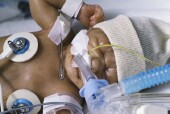 THURSDAY, Aug. 21 (HealthDay News) -- Dawn Marie Perkins wasn't even seven months pregnant with her twin boys when she knew something had gone terribly wrong.
After numerous tests and evaluations, Perkins quickly learned that strokes aren't something that just happens in the elderly; they can even strike an infant still in the womb.
Her son, Elijah Perkins, experienced a hemorrhagic stroke before he was born. It's not as rare as many might think. An estimated one out of every 4,000 babies born in the United States will have a stroke before they're 28 days old, according to new guidelines issued by the American Heart Association on managing childhood stroke.
"Most people do not think that young people have strokes," said Dr. Jose Biller, one of the authors of the new guidelines and chairman of the department of neurology at Loyola University Health System in Chicago. "But the point people should really understand is that they can occur in utero, they can occur in the neonatal period, and they can occur in older children. There are noticeable differences in presentation, risk factors, and the prognosis in children compared to older adults, however," Biller added.
Perkins said people are almost always surprised when she tells them about what happened to her son. "People are like, 'Kids don't have strokes.' So, I still think there's a lot of work to be done in terms of awareness," she said.
One of the biggest differences between childhood strokes and those that happen in older people is that far fewer of strokes in children are what's known as ischemic strokes. In an ischemic stroke, the blood supply to the brain is cut off, sometimes by a blood clot or possibly due to sickle cell disease. Without blood, the brain can't get the oxygen it needs to survive. Ischemic strokes are the most common in adults, according to Biller, accounting for 80 percent to 85 percent of strokes. In people under 18, about 55 percent of strokes are ischemic.
About 45 percent of strokes in children are hemorrhagic. Hemorrhagic strokes occur when a blood vessel in or on the brain bursts, causing blood to pool in the brain and depriving it of oxygen.
Some of the risk factors for stroke in childhood include sickle cell disease, heart disease, trauma and certain infections, according to the AHA guidelines, which were expected to be published in the September issue of Stroke.
Symptoms include:
- Sudden weakness or numbness occurring on the face, arms or legs, especially if it's one-sided.
- Sudden difficulty speaking or understanding what's being said.
- Confusion.
- Sudden trouble walking or a loss of balance.
- Dizziness.
- Sudden vision loss or difficulty seeing.
- Severe, sudden-onset headache.
As with adults, the prognosis for children varies. Generally, the faster you can get your child to the hospital, the better the prognosis, though not all of the treatments available to adults are available for the treatment of children. Perkins' son is almost 6 and has had to undergo years of physical and occupational and vision therapy, and he still has weakness on his right side, but Perkins said her son has made incredible progress, even more than doctors expected he would.
"The prognosis at the beginning wasn't very good. Eighty-five to 90 percent of the brain tissue on his left side is gone. The doctors thought he'd be in a wheelchair, that he'd never be able to walk or talk. He struggles a bit, and it may take him a little longer, but he does it all now," Perkins added.
More information
To learn more about stroke in children, visit the American Heart Association  . .
|  |

Exercise Reduces Blood Pressure...

THURSDAY, Aug. 14 (HealthDay News) -- For people with high blood pressure, exercise can be the most important lifestyle change they can make, researchers say.
Yet two-thirds of doctors don't take the time to tell their patients with high blood pressure about the importance of exercise and physical activity, a new study finds.
"Patients do follow physician recommendations to exercise when instructed to, and patients who follow exercise recommendations tend to have lower systolic blood pressures than those who do not," said lead researcher Dr. Josiah Halm, a hypertension specialist at the University of Wisconsin School of Medicine and Public Health.
The findings are published in the summer issue of Ethnicity & Disease.
For the study, Halm's team collected data on 17,474 people who participated in the Third National Health and Nutrition Examination Survey. Among these people, 4,686 reported having high blood pressure.
The researchers found that only slightly more than one-third of the people with high blood pressure said their doctor had told them to increase physical activity as a way of bringing down their blood pressure.
Yet, 71 percent of patients with high blood pressure saw a drop in their blood pressure when they increased their physical activity, which means that they listened when doctors told them to exercise more, according to the report.
"Non-pharmacological methods such as exercising are important in improving blood pressure control on a population level as this study looked at the cross-section of the U.S. population," Halm said.
Studies have shown that small changes in blood pressure -- 2 to 3 mmHg -- could result in a 25 percent to 50 percent decrease in the incidence of high blood pressure, also known as hypertension, Halm said. "That would result in an annual reduction of stroke, coronary heart disease and all-cause mortality by 6 percent, 4 percent and 3 percent, respectively," he said.
Exercise -- as part of a comprehensive lifestyle-modification program including weight loss, low-salt diet, diets rich in fruits and vegetables and low in saturated fats -- has beneficial effects on blood pressure, Halm said.
"It is thus appropriate to recommend exercise as most patients will follow their physician recommendations and this is associated with improved blood pressure control and likely a reduction in the morbidity and mortality associated with uncontrolled blood pressure," he said.
Dr. Gregg C. Fonarow, a professor of cardiology at the University of California, Los Angeles, thinks more needs to be done to get patients to make lifestyle changes that will reduce their blood pressure.
"Despite clinical trial evidence and national guideline recommendations for exercise counseling to be provided for patients with high blood pressure, this study demonstrates that only one-third of these eligible patients received exercise counseling," he said.
"Much more needs to be done to ensure that patients with high blood pressure receive appropriate counseling on lifestyle change -- including counseling on the importance of regular aerobic exercise -- from their physicians," Fonarow said.
More information
For more on high blood pressure, visit the American Heart Association  . .
|  |
|