| Background
In 2004, the Health Services and Resources
Administration (HRSA) issued a Request
for Proposals for a two-year research
project to gather information and insights
in support of the development of a new
methodology for identifying health care
facilities and communities with critical
shortages of registered nurses (RNs).
HRSA’s decision to support this research
was based in large part on their concern
that its current method for identifying
facilities and communities with shortages
of RNs was too narrow in scope and that
RN shortages were likely to worsen over
the next 20 years. The New York Center
for Health Workforce Studies at SUNY Albany
was selected to conduct this study.
This report summarizes the findings of
the various components of this empirical
research study. It describes a number
of methods for identifying facilities
and communities with shortages of nurses.
It documents the strengths and weaknesses
of different methods for assessing the
extent of shortages of RNs in facilities
and communities. The report is presented
in seven sections, each summarizing a
different aspect of the study:
- Federal Initiatives to Address Nursing
Shortages
- Initial Literature Review
- Data Sets and Compilations
- Methods and Analyses Based on Facility
Data
- Methods and Analyses Based on Geographic
Data
- Preferred Method
- Study Recommendations
In addition to summarizing these research
components of the study, this report presents
a series of conclusions designed to inform
policy makers and other researchers who
may be interested in implementing or adapting
one or more of these methods in the future.
Additional details about the different
methods, including estimates of the supply
and demand for RNs in different jurisdictions,
can be found in the technical report prepared
as part of the larger study.
A. Federal
Initiatives to Address Nursing Shortages
The Federal government has had a long-standing
interest in the nursing workforce. For
more than two decades, through its National
Center for Health Workforce Analysis,
Division of Nursing and the Shortage Designation
Branch of HRSA has collected data on nurses
in the U.S. and developed quantitative
models to estimate the current and future
supply of and demand for RNs. Several
programs to encourage new RNs to practice
in facilities and communities with severe
shortages of RNs, including the Nursing
Education Loan Repayment Program (NELRP)
and the Nursing Scholarship Program, have
been operating for many years. These programs
help to alleviate persistent shortages
of RNs.
In framing the parameters for this research
study, HRSA identified a number of issues
that needed resolution including:
- Should indicators developed to measure
critical shortages of RNs be based
on need for RNs or demand
for RNs?
- Can standard indicators that measure
critical shortages of RNs be applied
to all of the eligible settings [1]
included in this study?
- Can variations in the supply of
and demand for RNs by region, geography
(i.e., rural or urban), setting, or
facility be accounted for in indicators
that measure RN shortages?
- Are setting-specific data sets
available at the national level that
include the elements needed to measure
critical shortages of RNs?
- Can a process be developed that
identifies facilities with the most
serious shortages of RNs so that Federal
resources can be targeted to the neediest
facilities?
- How can true shortages of nurses
be distinguished from shortages created
by poor management practices?
An effective study should take all of
these issues into account while researching
and testing the development of a national
methodology to measure shortages of RNs.
Current methods are inadequate. A better
method would support several government
incentive programs to attract new nurses.
It would also provide a better basis for
monitoring RN shortages locally and nationally.
One important Federal response to the
national nursing shortage was the Nurse
Reinvestment Act, which was enacted in
August 2002. The Act reauthorized the
NELRP, which provides loan repayment to
RNs in return for work at facilities or
in communities with a shortage of RNs,
and established the Nursing Scholarship
Program. Eligible placement sites for
these programs were expanded to include:
- Ambulatory surgical centers;
- Federally designated migrant, community
public housing, or homeless health centers;
- Federally qualified health centers;
- Home health agencies;
- Hospice programs;
- Hospitals;
- Indian Health Service centers;
- Native Hawaiian health centers;
- Nursing homes;
- Rural health clinics; and
- State or local health department clinics
or skilled nursing facilities.
The method used for the identification
of qualified placement sites included
a combination of geographic and facility
designations. In 2002, the New York Center
for Health Workforce Studies assisted
the Bureau of Health Professions by developing
an up-to-date list of nursing shortage
hospitals and counties throughout the
U.S. and its territories. The Center used
two separate methodologies, one to identify
private, non-profit hospitals with shortages
of nurses and the second to identify counties
with shortages of nurses. Appendix C of
the full technical report provides a brief
description of the methodologies used
for the designation of hospitals and areas
with nursing shortages.
Because this approach relied on hospital
nursing data to identify facilities with
nursing shortages, it failed to quantify
nursing shortages experienced by any providers
except hospitals. Most of the other types
of facilities included on the list above
were considered categorically eligible,
based on the premise that they faced critical
shortage of nurses.
B. Study Overview
In the general context described
above, this study was conducted over a
two-year period, starting in the fall
of 2004. After a brief summary of the
study goals, objectives, and other characteristics
of the study, the ten study components
are summarized below.
1. Project
Goals and Objectives
The primary goal of this study was to
conduct research on the necessary components
of a comprehensive, nationwide methodology
to identify facilities and communities
with critical shortages of RNs across
the U.S. and its territories in order
to target the placement of Federally-obligated
RN scholars and loan repayers. This research,
which involved statistical analysis supported
by expert opinion, took into account population
needs, practice settings, appropriate
staffing levels, and nursing education,
among other aspects of the supply of and
demand for RNs. As a secondary benefit,
the project revealed important insights
about the differences in the use and distribution
of RNs across the various settings and
geographic areas of the country.
The study’s staff worked to achieve the
following objectives in support of the
primary goal of the study:
- Identify and define indicators and
measures that reflect critical RN shortages
for the four types of facilities;
- Assess the availability of data sets
that can be used to determine RN staffing
needs nationally in each of the settings
listed above;
- Develop quantifiable key measures
of nursing shortages based on key indicators
described above as well as the available
data sets that include the necessary
data to calculate the key measure.
- Determine whether these key measures
of shortage can be incorporated into
a comprehensive national methodology
to identify facilities and agencies
with critical nursing shortages based
on the following criteria:
- the measure accurately quantifies
nursing shortages in a specific
health care setting; and
- the measure either can be calculated
using an available national data
set or the data can be collected
and validated at the facility level.
- Establish an analytic framework that
can be used for a comprehensive methodology
to determine critical nursing shortages
across a variety of health care settings.
Ultimately, this research will support
the development of a comprehensive method
for identifying the health care facilities
and agencies with critical shortages of
RNs. This will permit more effective targeting
of Federal and other resources to encourage
service-obligated RNs to work in the facilities
and communities with the greatest needs.
2. Expert Advisory
Panels
The study was conducted under the guidance
of four expert advisory panels, one for
each of four types of health care organizations:
hospitals, home health agencies, nursing
homes, and public health agencies. The
names of the panelists can be found in
Appendix B of the full, technical report.
These panels met face-to-face twice.
The first meetings were held separately
early in the study to discuss preliminary
findings and agree on strategies for accomplishing
study goals and objectives. The second
meeting convened all the panels together
toward the end of the study to gain the
benefit of cross-fertilization of ideas.
In between these meetings the panelists
were invited to participate in two conference
calls in which interim progress reports
were provided to solicit feedback and
suggestions.
An important outcome of the initial meetings
of the advisory panels was agreement on
a list of “guiding principles” to inform
and direct our efforts. These principles
can be roughly classified as relating
to theoretical, practical, or fairness
concerns. The list also included some
specific recommendations about methodology.
The theoretical principles and ideals
included:
- Context: facility within community.
Both facility and community characteristics
must be considered, but community characteristics
are more important than facility characteristics.
- Demand over need. Analyses
should primarily focus on employer demand
for RNs (e.g., what the local labor
market will actually support) rather
than the health needs of the population.
High-need areas that have no resources
or infrastructure to employ additional
RNs would find little benefit in the
NELRP program.
- Identify standards for data.
Ultimately, it will be important to
upgrade Federal, state, and local data
systems to support better planning for
the nursing workforce, including the
designation of facilities and communities
with shortages of RNs.
- Consider facility culture.
Some facilities may experience high
RN vacancies not because of difficulties
recruiting RNs, but because of persistent
RN turnover due to problems of organizational
culture within the facility (e.g., poor
management). This is not a “shortage”
issue, and the NELRP program is not
intended to address such problems.
- Define shortage based on outcomes.
Theoretically, a facility can be said
to have “too few” RNs when there are
not enough RNs for the facility to effectively
function. This will be observed in certain
outcome measures relating to quality
of care and facility functioning.
The principles and ideals relating to
practical concerns included:
- Low administrative burden on facilities
and HRSA. Data used in the final
methodology should not require a large-scale
data collection or manipulation.
- Applicable to all facility types.
The final shortage methodology should
be applicable to and appropriate for
all facility types.
- Readily available data over time.
Ideally, the final methodology should
be supported by existing data that are
easy to access and available over time
for updating.
- Commonly accepted data elements
and indicators. Using established
indicators of supply, demand, and shortage
is preferable to developing new ones.
- Easy to update to reflect changing
environment. Data used for identifying
shortages should be easy to update so
that designations can be periodically
reexamined.
The principles and ideals relating to
fairness included:
- Attention to rural and urban differences.
The shortage designation method should
not systematically disadvantage either
rural or urban facilities.
- Special needs of some facilities.
The shortage designation method should
recognize extenuating circumstances
(e.g., facing critical problems, serving
special populations).
- Case mix of patients. The
method should recognize that some facilities
have higher patient acuity than others,
which may signify that some facilities
require more intensive staffing.
- Accommodate data manipulation.
The method should minimize opportunities
for facilities and communities to “game”
the system to achieve a shortage designation.
Specific recommendations for the method
included:
- Look beyond clinical care.
It should be recognized that overall
demand for RNs extends beyond just those
at the bedside to those in non-clinical
positions.
- Consider overall staff mix.
Some employees may substitute for RNs
with other personnel. This may be more
or less appropriate depending upon the
facility type.
- Consider RN staff mix (e.g.,
specialty, education). Facilities with
enough RNs overall may still have a
shortage of RNs with certain credentials
or in some services (e.g., ICUs).
- Separate out different units within
hospital care. Different units have
different staffing needs (e.g. intensive
care units will require more RNs than
general medical-surgical units).
Most of these guiding principles were
addressed in at least some of the analyses,
either directly or indirectly, and many
are incorporated into the Preferred Method
proposed by the study.
3. Characteristics
of an Ideal Shortage Designation Method
Early in the study a number of characteristics
were identified as especially desirable
for any method to identify facilities
and communities with shortages of RNs.
These characteristics, some of which may
not be attainable, included:
- A common method to be used across
the nation;
- Ease of calculation of the RN shortage
index for individual facilities and
communities;
- Implementation using existing data
sets, with no additional data collection
required;
- Comparison of shortages of RNs both
within and between different types of
facilities;
- Comparison of RN shortages across
different states and other geographic
jurisdictions;
- Consistency of shortage severity estimates
with shortage assessments by local experts;
- Identification of shortages in facilities
due to poor management; and
- Easy updates to the method to reflect
more recent conditions, situations,
and relationships.
C. Initial
Literature Review
The first component of the research involved
a careful review of the literature, focusing
on characteristics of RNs relevant to
the task of understanding current and
future shortages. The discussion that
follows summarizes a variety of relevant
statistics.
1. Characteristics
of RNs
- Table 1 shows that although 6.1% of
RNs were men in 2004, which is higher
than in previous years, nursing remains
a female-dominated profession. This
means that, at least in the near future,
recruiting more men to the profession
is not likely to be an important avenue
for increasing the supply.
- By 2014 it will be necessary to recruit
more than 400,000 new RNs just to replace
those RNs older than age 55 who are
expected to retire from active nursing
practice.
- The latest estimates developed by
the Bureau of Labor Statistics [BLS,
2006] indicate that the U.S. will require
1.2 million new RNs by 2014 to meet
the nursing needs of the country, 500,000
to replace those leaving practice and
an additional 700,000 to meet growing
demands for nursing services.
Table
1. Active RNs in the U.S. by Gender and
Age Group, 2004
| Age
Group |
Male |
Female |
Percent |
| <
25 |
1,731 |
57,843 |
2.5% |
| 25
to 29 |
10,955 |
148,721 |
6.7% |
| 30
to 34 |
15,508 |
205,543 |
9.2% |
| 35
to 39 |
19,217 |
237,693 |
10.7% |
| 40
to 44 |
23,951 |
336,195 |
15.0% |
| 45
to 49 |
30,986 |
418,634 |
18.8% |
| 50
to 54 |
24,098 |
382,650 |
17.0% |
| 55
to 59 |
13,469 |
257,640 |
11.3% |
| 60
to 64 |
4,909 |
131,281 |
5.7% |
| 65
+ |
1,819 |
73,486 |
3.1% |
| Percent |
6.1% |
93.9% |
2,396,329 |
Source: 2004 NSSRN
2. Employment
Settings
- In 2004, more than 57% of RNs worked
in hospitals, 11% worked in public or
community health, nearly 12% worked
in ambulatory care settings, and almost
7% worked in nursing homes and extended
care facilities (Figure 1).
Figure
1. RN Employment by Setting, 2004
 [D] [D]
Source: The Registered Nurse Population,
March 2004. USDHHS, Bureau of Health Professions,
Division of Nursing, November 2005.
3. Trends in
Supply
- Between 1980 and 2004, the number
of active RNs in the U.S. grew by nearly
90%. In 2000, there were more than 2.4
million active RNs, an increase of more
than 1.1 million over 1980.
- Between 1996 and 2000, the total
number of RNs grew by only 1.3% each
year, compared with average annual growth
of 2% to 3% in earlier years (Figure
2). This slowdown in growth between
1996 and 2000 is attributable to two
trends: a declining number of candidates
passing the RN licensing examination
annually and an increasing number of
RNs leaving the field [1].
This slowdown was temporary, however,
as the growth in the supply of RNs of
early years resumed between 2000 and
2004, more than keeping up with the
growth in the population over the same
period.
- The number of candidates passing the
RN licensure examination has decreased
steadily since 1995. Between 1995 and
2001, the number of RNs passing the
licensing exam declined by nearly 28%
[2].
Figure
2. Active RNs per 100,000 Population,
U.S., 1980 to 2004
 [D]
[D]
Sources: U.S. Department of Health and
Human Services, National Sample Survey
of RNs, 2004 and earlier; Population Estimates
Program, Population Division, U.S. Census
Bureau.
- Between 1995 and 2001, the number
of graduates of RN education programs
in the U.S. declined. Nearly 29% fewer
RNs graduated in 2001 than in 1995 [2].
The numbers of RN graduates have been
steadily increasing since 2002 and in
some states, including New York, they
are now higher than the previous peak
number in 1996 [3,
4].
There is evidence capacity limits in
many nursing education programs (due
to such factors as the inability to
recruit enough faculty) are limiting
the ability of the system to accept
all qualified nursing school applicants.
4. Geographic
Distribution
The geographic dispersion of active RNs
in 2004 was far from uniform across the
U.S. In fact, Figure 3 shows that the
ratio of the highest to lowest RN per
capita ratios was nearly 4:1, with the
highest ratios in the District of Columbia
(2,236 RNs per 100,000 population) and
New Hampshire (1,321), and the lowest
in California (603) and Nevada (612).
Figure
3. RNs per 100,000 Population in the U.S.,
2004
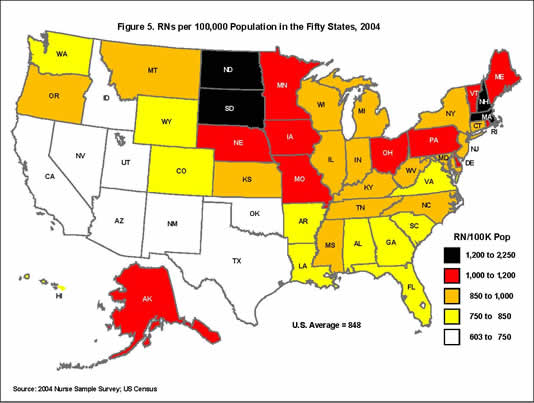 [D] [D]
5. Projections
of Future Supply
- A growing shortage of RNs has been
projected over the next 15 fifteen years,
with a 12% shortage by 2010 and a 20%
shortage by 2015 (Figure 4). The projected
shortage is the result of the expected
increase in demand coupled with a relatively
stable supply of RNs [5].
- Figure 5 updates these projections
based in part on the 2004 National Sample
Survey of Registered Nurses (NSSRN).
Total numbers of RNs may rise until
2016 if age-specific cohorts follow
patterns observed in the NSSRN between
2000 and 2004. This is in large part
because the sizes of birth cohorts in
nursing tend to increase well into ages
50-55, and so a number of baby boomers
(currently ages 43 to 60) may still
enter nursing as a second career over
the next 10 years.
- This does not mean that problems will
not be felt until after 2016, however.
Using these projections of numbers of
RNs and projections of the total population
and the population age 65 and older
from the U.S. Census Bureau, Figure
5 shows that the number of RNs per 100,000
population will peak in 2012, while
the number of RNs per 100,000 population
age 65 and older will peak in 2008 and
decline by 5% (falling below current
rates) by 2012.
Figure
4. National Supply and Demand Projections
for RNs, 2000 to 2015
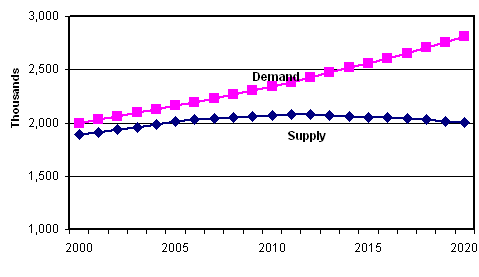 [D]
[D]
Source: Bureau of Health Professions,
RN Supply and Demand Projections
Figure
5. Indexed Projections of RNs per 100K
Population, RNs per 100K Age 65+ Population,
and Projected Numbers of Active RNs, 2004
to 2024
 [D] [D]
Source: CHWS, 2006
6. Nursing
Shortages
A review of the literature revealed a
number of studies examining future shortages
of RNs relevant to this study. Some of
the key findings are summarized briefly
below.
- Health care providers across a variety
of settings reported increasing difficulty
recruiting and retaining RNs, particularly
in hospital settings [6,
7].
- There were indications that the attrition
from clinical settings may be related
to dissatisfaction with working conditions.
The 2004 NSSRN asked RNs about job satisfaction
and found that 76% of RNs employed by
hospitals and 75% of RNs employed by
nursing homes were satisfied with their
jobs, compared to 82% of RNs employed
in nursing education and 83% of RNs
employed in occupational health.
- There is growing concern about the
impact of RN shortages on the quality
of health care. A growing body of evidence
demonstrates that hospitals with lower
ratios of RNs to patients had more adverse
events than hospitals with higher RN
to patient ratios [8,
9, 10].
|